Restoring hope, rebuilding lives: A day in the life of a fistula surgeon in Zambia
NORTH-WESTERN PROVINCE, Zambia – Around the world, half a million women and girls are thought to be living with obstetric fistula, a serious childbirth injury that can cause incontinence and result in significant medical and mental health issues. In Zambia, as of 2018, more than 33,000 women and girls had been affected.
For over a decade, the Government of Zambia and UNFPA have partnered to provide fistula survivors with life-transforming surgeries aimed at healing their physical and psychological wounds. Many of these procedures are conducted at fistula camps held at Zambia’s main provincial hospitals, where three or more doctors gather to perform surgeries for several days.
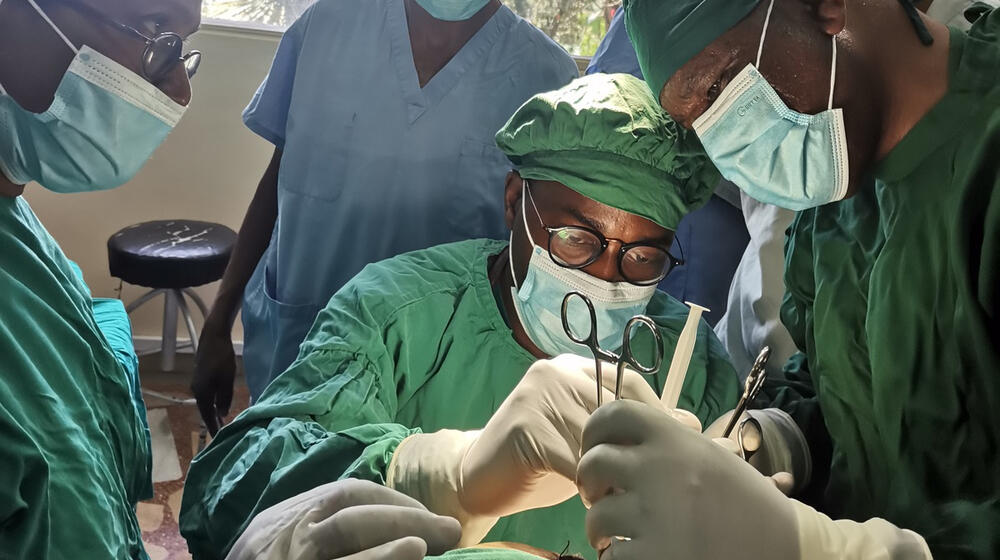
Dr. Paul Musoba is one of just eight fistula surgeons in the country. On the occasion of the International Day to End Obstetric Fistula, UNFPA sat down with Dr. Musoba, who works at the Solwezi general hospital in Zambia’s North-Western Province, to learn more about what drew him to this field of surgery, the challenges he encounters in his work and the successes that have made him proud to be a fistula surgeon. This interview has been edited and condensed.
What inspired you to become a fistula surgeon?
Early in my practice as an obstetrician and gynaecologist, I encountered many women and girls who had suffered greatly from obstetric fistula. Seeing women and girls abandoned and ostracized due to their constant leakage of urine, faeces or both was the starting point of my desire to change the narrative.
Taking inspiration and mentorship from some of Zambia’s senior fistula surgeons, I first participated in a fistula camp in 2019. I was able to observe, assist and eventually undertake fistula surgeries. It is definitely a specialized skill that requires constant practice and exposure.
It is quite fulfilling, but at the same time, challenging.
Can you talk about the scope of the problem of fistula in Zambia?
Pregnancy and childbirth should be among the happiest times in a woman’s life. Sadly, this is not the case for thousands of women and girls not only in North-Western Province, where I am located, but across Zambia at large.
At the Solwezi general hospital, I often encounter women and girls who have developed obstetric fistula, some of whom have lived with the condition for years.
How do you approach meeting the specific needs of fistula patients?
My journey begins with me getting to understand their situation. The trauma suffered by many of my clients during delivery is heartbreaking, as it goes beyond the physical. I focus throughout not only on healing their physical wounds, but also supporting their emotional and psychological healing.
During fistula camps, my surgical work typically begins at 7:30 a.m. and ends at 6 p.m., with 15-minute intervals in the operating theatre between clients. This maximizes on time against high demand.
The process concludes with a hospital discharge of a happy, “dry” and “continent” client. It makes me proud to be a fistula surgeon.
What are some of the challenges you face while working to support women and girls affected by fistula?
Every year, I repair an average of ten fistula clients, at either the Solwezi general hospital or during fistula camps at other hospitals. However, I know there are many other women suffering with fistula who are not able to access treatment due to lack of information or challenges in accessing health care.
Getting to expectant mothers, as well those suffering from fistula in their communities, is therefore one of the biggest challenges I face. Many women in North-Western Province live in remote areas located far from health facilities, often resulting in home deliveries – a key risk factor for obstetric fistula in the event of obstructed labour.
Additionally, for many fistula survivors, societal stigma still remains a major issue. Successful reintegration is a key priority post-surgery.
Can you share a story from your work with fistula patients that has stuck with you?
My recent encounter with an 18-year-old fistula survivor stands out to me. She developed obstetric fistula due to obstructed labour and delayed access to emergency health care, and lost her baby.
For two years she lived with fistula and could not continue with her education. But with the help of community health workers, she was able to access surgical care, and I successfully repaired her fistula.
Throughout this process, she was very jovial and optimistic; her confidence put pressure on the team. I personally made a follow-up visit four months after her operation, and the girl we had discharged had an even brighter smile.
She told me: “Dr Musoba, thanks to you, I have now gone back to school and am looking forward to completing my education!”