News & Updates
Obstetric fistula stories and announcements
Obstetric fistula stories and announcements

Statement of UNFPA Executive Director Dr. Natalia Kanem on the International Day to End Obstetric Fistula, 23 May 2019
Learn more
Statement of UNFPA Executive Director Dr. Natalia Kanem on the International Day to End Obstetric Fistula, 23 May 2019
Shame, isolation and segregation are among the indignities faced by the hundreds of thousands of women and girls worldwide who suffer from obstetric fistula, an injury of the birth canal after prolonged and obstructed labour. The girls and women afflicted by the condition, which is preventable and largely treatable, are often plagued by chronic incontinence. As a result, they face devastating social stigma.
The majority of women and girls who suffer from fistula are poor. Their inability to receive prompt medical treatment not only deprives them of their health and dignity, but is a violation of their human rights.
UNFPA leads the Campaign to End Fistula. Since 2003, UNFPA has supported over 100,000 fistula repair surgeries, and campaign partners have supported thousands more, enabling women and girls in more than 55 countries across Africa, Asia, the Arab region and Latin America to regain hope and rebuild their lives.
One survivor, Nasiwelo Bisolomo, lost her baby at the age of 18 after a prolonged obstructed labour at home. She suffered from fistula for the next 46 years. She nearly had lost all hope when she heard of a UNFPA-supported fistula camp and travelled 300 km to undergo the life-transforming healing surgery. Now, she is helping spread the word that fistula treatment is available.
It is time for the world to heed the call made by United Nations Member States in the 2018 United Nations Resolution on Ending Fistula in which they committed to eradicating the condition within a decade. Yet, achieving this goal requires increased investments, innovations and partnerships. Failure to take action will undermine our chances of achieving the Sustainable Development Goals, meeting the commitments of the International Conference on Population and Development, and ensuring no one is left behind.
No woman or girl should be deprived of her dignity, hopes and dreams. Fistula is a human rights violation – end it now!
Fistula is a sad, shameful and isolated life of over two million women around the world.
Watch the videoFistula is a sad, shameful and isolated life of over two million women around the world.

DHARAN, Nepal – At the age of 17, Palesh Devi Rajdhobi was married off to a man she had never met. One year later, she gave birth to her first child. Then another, and another. When she was pregnant with her sixth, she knew something was wrong.
Read MoreDHARAN, Nepal – At the age of 17, Palesh Devi Rajdhobi was married off to a man she had never met. One year later, she gave birth to her first child. Then another, and another. When she was pregnant with her sixth, she knew something was wrong.
“By the time I was taken to the hospital, it was already too late. Two tragedies befell me. I had a stillbirth and started leaking urine constantly,” Ms. Rajdhobi told UNFPA.
After a prolonged labour, she had developed an obstetric fistula, a hole in the birth canal that renders women incontinent, unable to control their urine, faeces or both. Left untreated, the condition can cause infection, pain and a host of other problems – including social isolation and depression.
“I was thinking that I would leak urine throughout my remaining life and there was no cure for my suffering. I was always ashamed to leave the house because of the smell,” Ms. Rajdhobi said.
Fistula is one of the most serious childbirth injuries. And it is almost entirely preventable.
With access to maternal health care – particularly, caesarean sections – the injury has been largely eliminated in much of the world.
Yet it still afflicts the most marginalized women and girls, those without the money or ability to receive quality obstetric care. Girls who become pregnant too early, such as child brides, are especially vulnerable.
Today, more than 2 million women in the developing world are estimated to be living with the condition.
“Nobody would insist on visiting health centres for pregnancy check-ups back then,” Ms. Rajdhobi explained. “There were no means of transportation. We had to walk at least four hours to reach the nearest health facility.”
For more than two decades, Ms. Rajdhobi lived with fistula.
The social isolation she suffered as a result was particularly unbearable. Instead of going to the market and visiting friends and family, she was confined to the privacy of her home, too distraught to encounter community members who spoke ill of her.
She is not alone.
Nara Maya Rai, now 64, was left with the debilitating childbirth injury after her third pregnancy.
“[Back in] that time,” she recalled, “a pregnant woman in our village had to be carried four hours in a bamboo basket, and then three hours in a vehicle if she were to be taken to a hospital.”
Ms. Rai lives roughly 400 kilometres from the nearest large city. After developing an obstetric fistula, she, too, was ostracized from her community. “When I would go close to a village assembly, some of them would cover their noses and ask where that bad smell emanated from. I would wash my clothes several times a day.”
These stories are all too common – in Nepal and throughout the developing world. According to UNFPA data, an estimated 50,000 to 100,000 new cases of obstetric fistula develop each year.
As the leader of Campaign to End Fistula, UNFPA provides technical guidance, medical supplies, training and funds for fistula prevention, treatment and social reintegration programmes. UNFPA also strengthens reproductive health care and emergency obstetric services to prevent fistula from occurring.
In Nepal, UNFPA is supporting BP Koirala Institute of Health Sciences to provide free surgery and post-operative care to women who live with the injury. Over 30 women have already received treatment, of an estimated 200 to 400 who suffer from fistula each year in Nepal.
UNFPA is also working with its partners to raise awareness of the condition.
“In rural areas, many women and girls living with fistula do not receive any family support and never seek treatment, because they don’t know what is wrong with them and where to seek service,” said Maiya Bhattarai, a community mobilizer who orients women on obstetric fistula.
“We particularly engage women who are hard to reach, such as those living in rural areas and who are poor,” she said.
Ms. Rajdhobi and Ms. Rai are two of the women to receive free reconstructive surgery from the UNFPA-supported campaign in Nepal.
For them, life without fistula brings more than freedom from pain. It brings freedom from isolation.
“It was like walking out of prison," Ms. Rajdhobi said, still remembering the day she left the hospital. "I was in tears of happiness.”
– Santosh Chhetri

SANA’A, Yemen – Najat, a trained midwife, was well aware of the dangers of pregnancy and childbirth. But when her own health needs and professional judgment clashed with her husband’s traditional ideas, she suffered in ways she could not have imagined.
Read MoreSANA’A, Yemen – Najat, a trained midwife, was well aware of the dangers of pregnancy and childbirth. But when her own health needs and professional judgment clashed with her husband’s traditional ideas, she suffered in ways she could not have imagined.
Najat was a midwife in the Wesab area of Dhamar Governorate. When she got married, she moved to her husband’s village, and continued practicing midwifery – even riding a donkey to reach faraway patients.
“It was difficult in the beginning to cope with the new environment. But then I managed to build good relations with the villagers, and I started to provide midwifery services to women in the village,” she told UNFPA.
She delivered 36 babies in her new village, and encouraged women to give birth in the hospital when possible.
But her own family would not heed this advice.
Najat became pregnant in her first year of marriage, and was overjoyed. She sought regular check-ups to ensure the health of her pregnancy. When she learned the fetus was not in the proper position, the solution was clear: a Caesarean section delivery.
But her in-laws disapproved.
The family was conservative, and they had long objected to Najat’s midwifery practice. They felt maternal health services were indulgences.
When Najat insisted she needed hospital care, her mother-in-law intervened. “She told me that there was no need for the hospital. She had given birth to many children before and did not need the hospital,” Najat recalled. The family regarded hospital care as “a mere luxury.”
As Najat feared, she went into a prolonged, obstructed labour, a potentially fatal condition for both mother and baby. She begged her husband and mother-in-law for help, but they ignored her – for days.
“I stayed for four days suffering from pain trying to give birth, but in vain,” she said. “My body was exhausted, and I was physically and psychologically worn-out.”
It was only when they saw she was on the brink of death that they reluctantly agreed to transport her to a hospital.
As soon as she arrived, an emergency C-section was performed. Miraculously, both Najat and her daughter survived.
But Najat’s ordeal was only beginning.
As she recovered from surgery, she discovered further complications. “I thought that an open water bottle behind me might have fallen and I did not notice it. Eventually, I realized the wetness was coming from me.”
She realized she had developed an obstetric fistula, a hole that develops when birth canal tissues die following a prolonged, obstructed labour. The condition causes incontinence, infections and social isolation.
Because it can be prevented with timely access to a C-section, the injury has been largely eliminated in much of the world. Today, it afflicts the most marginalized women and girls – those without the power, money or ability to receive emergency obstetric care.
The doctor confirmed her diagnosis.
Although she required further recovery, Najat’s husband and mother-in-law insisted she return to their village to resume her domestic duties.
“Thinking about the continuous leaking of urine and walking with the catheter was just embarrassing and humiliating in the presence of many of my sisters-in-law in the house,” Najat said.
“Who would accept me like that? Who would clean after me constantly? I also had my own daily home chores. That scenario was difficult to handle. So I decided not to go back to the village.”
Her husband returned to his village, taking their daughter with him.
Najat went to her parents' house. For months, her family tried to bring the baby back to see her, but their attempts failed.
Meanwhile, Najat learned about a UNFPA-supported fistula unit at the Al-Thawrah Hospital in the capital, Sana’a. “Through a WhatsApp group, I read the announcement about treating fistula cases for free. I contacted them,” she said.
Her family was able to raise the funds needed to transport her to the hospital. Finally, seven months after giving birth, she received a surgical fistula repair.
“I got treated, and here I am,” she told UNFPA.
Since 2011, the UNFPA-supported fistula treatment units in Sana’a and Aden have successfully treated nearly 290 cases of obstetric fistula.
Survivors, who often endure months or years of stigma, may also require assistance reintegrating into their communities. But Najat knew just how to resume her daily life.
She began working in a private hospital in Sana’a. Today, she is on a waiting list to receive UNFPA assistance to open up her own home-based midwifery clinic.
She is happy to be starting a new future, but her heart aches for the baby who was taken from her. “I cannot dream anymore,” she said.
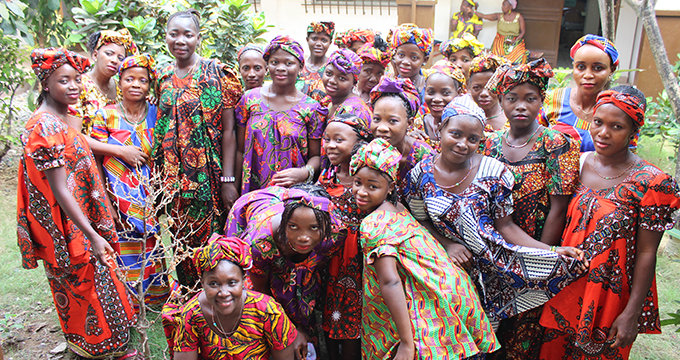
FREETOWN, Sierra Leone – “When I became pregnant in December 2016, I never attended a health clinic,” said 19-year-old Katimu Kanneh. “I drank traditional medicines supplied to me by traditional birth attendants in the community.”
FREETOWN, Sierra Leone – “When I became pregnant in December 2016, I never attended a health clinic,” said 19-year-old Katimu Kanneh. “I drank traditional medicines supplied to me by traditional birth attendants in the community.”
Ms. Kanneh’s labour was difficult, and without adequate care, her baby was stillborn. And her pain didn’t end there. “It was only after the delivery that I started leaking urine, and my life hasn’t been the same since,” she said.
The traumatic delivery left her with obstetric fistula – a hole between the birth canal and bladder or rectum resulting from prolonged, obstructed labour in the absence of timely medical treatment. Often, this serious injury leaves women incontinent, unable to control their urine, faeces or both.
“Some people in the community have associated my condition with witchcraft,” said Ms. Kanneh. Ostracized by her community and her husband, she left her home in the Kailahun District’s Malema chiefdom to seek treatment.
“For the last four months, my family have been unaware of my whereabouts,” she said.
According to UNFPA, an estimated 2 million women in Sub-Saharan Africa, the Arab States, and Latin America and the Caribbean regions live with fistula, with approximately 50,000 to 100,000 new cases every year. The obstructed labour that leads to the condition can cause severe disability or even death; in Sierra Leone, more than 3,000 women die each year as a direct result of obstetric complications.
Among women who live with fistula, Ms. Kanneh’s story of ostracism is an all too common one.
“The effects are much more than the physical pain,” said Aminata Jalloh, an obstetric fistula supervisor at Aberdeen Women’s Centre in Freetown. “The condition often leaves them rejected by their husbands, stigmatized by their families, and alienated by their communities.” The discrimination often drives women from their homes and puts their livelihoods in jeopardy.

Entirely preventable with emergency obstetric care that enables women to deliver by Caesarean section, fistula is also treatable. With funding from UNFPA, the Aberdeen Women’s Centre runs a two-week fistula camp providing free surgery and post-operative care to patients from all districts of Sierra Leone.
But the same stigmatization that isolates fistula survivors within their communities can keep them from seeking treatment.
“It’s quite challenging getting patients to come for screening because of the stigma surrounding fistula,” said Alie Kamara, fistula programme officer at the Aberdeen Women’s Centre. “Many of them are not confident to leave their homes to get screened.”
To overcome the stigma and get women and girls the treatment they need, Haikal, a non-governmental organization and UNFPA partner, has mobilized previous fistula repair patients to serve as ‘fistula champions’ – living testimonies of what treatment can accomplish. The champions help identify women and girls living with fistula, encourage them to get screened, and refer them for treatment.
In 2018, UNFPA plans to support the Aberdeen Women’s Centre to perform 175 surgeries. Ms. Kanneh, referred by Haikal, was one of 56 women and girls living with obstetric fistula who recently attended the camp.
Before her healing could begin, though, she was in for yet more pain and shock: the screening revealed further damage sustained during her delivery.
“The doctors said I can no longer have babies because my uterus was removed without me knowing,” Ms. Kanneh said. To help her cope with the anguish, the Centre provided psychosocial counselling.
It is not uncommon for the screening done prior to fistula treatment to identify other pelvic, uterine or vaginal conditions. “When a client is screened for fistula, and you see how the condition has damaged their birth canal or bladder, you want to ensure you do your utmost to help them regain their dignity,” said Ms. Jalloh.
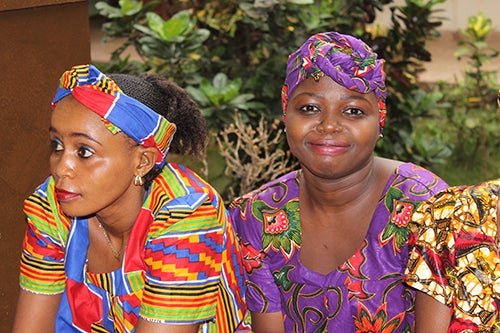
“When I think of 19-year-old Katimu who can no longer give birth, it makes me realize I have an important role to play in helping these women recover, so they can truly live their lives,” she added.
Treatment at the fistula camp does not end with the surgeries and post-operative medical care. As in Ms. Kanneh’s case, fistula survivors can benefit from counselling to help them cope with their condition and its impact on their bodies and their lives. Haikal also provides them with wellness kits containing clothing, medicines and hygiene supplies, and – to help them reestablish their lives and reintegrate into their communities – offers technical and vocational training as well as small grants to fund start-up enterprises.
“I can’t wait to go home to reunite with my family and restart my life,” said Ms. Kanneh.

MULANJE DISTRICT, Malawi – Margret Rambiki was just a teenager, married at 14, when she nearly died in childbirth.
It was 2002 in the Mulanje District of southern Malawi. A child bride, Ms. Rambiki may have been physically unready for pregnancy.
Read MoreMULANJE DISTRICT, Malawi – Margret Rambiki was just a teenager, married at 14, when she nearly died in childbirth.
It was 2002 in the Mulanje District of southern Malawi. A child bride, Ms. Rambiki may have been physically unready for pregnancy.
Her labour was prolonged and obstructed, a potentially deadly complication. And her access to emergency care was dangerously delayed. She remembers her father arguing with the health care provider because of their long wait for assistance.
Tragically, the baby was stillborn, and Ms. Rambiki was left with an obstetric fistula – a hole in the birth canal – that left her incontinent and vulnerable to a host of other medical concerns, including infections.
“I never enjoyed being a woman since I had this condition,” she later recalled. “It was tough to live.”
Today is the International Day to End Obstetric Fistula. Fistula is one of the most serious and tragic childbirth injuries, and it is almost entirely preventable. Access to proper maternal health care, particularly Caesarean sections to treat obstructed labour, can save the lives and health of both women and their babies.
Yet more than 2 million women in the developing world are estimated to be living with this condition. Its persistence is a sign that health and protection systems are failing women and girls.
Ms. Rambiki lived with obstetric fistula for 13 years. In that time, she had a son and a daughter. But, like many fistula survivors, she was isolated, enduring ridicule if she left home. She was unable to do community work, attend funerals or visit church, she told UNFPA.
And nothing seemed to help. “Traditional herbalists tried everything, and we had been told to do lots of things but the condition was never healed,” she recalled. “When you are in that situation, you try almost everything.”
But one day three years ago, her mother was chatting with neighbours at a nearby borehole. Someone mentioned that a woman in the district had received treatment for chronic urinary incontinence. It turned out a fistula repair camp was taking place at Mulanje district hospital.
She rushed to tell her daughter.
Over 25 women received treatment during the UNFPA-supported event, including Ms. Rambiki.
“I am now dry. I have no problem,” Ms. Rambiki said. “This is how a woman should be.”
Many of the women, like her, had endured the condition a long time. One lived with fistula for 66 years.
It is estimated that 1 per cent of women in the country have experienced an obstetric fistula, according to a 2016 survey.

UNFPA has been working with the Government of Malawi, the Freedom from Fistula Foundation and AMREF Health Africa on fistula treatment efforts since 2011.
Earlier this year, UNFPA organized another fistula repair camp at Mulanje hospital, treating 28 women, and referring others for specialized treatment. Women from the surrounding districts of Blantyre, Chiradzulu, Neno, Phalombe and Thyolo, and from across the border in Mozambique, came to access the services.
“This treatment outreach approach has brought services significantly closer to the underprivileged women who suffer in silence while seeking treatment,” said Grace Hiwa, a fistula expert with UNFPA.
The camp also mobilized more than 60 women to raise awareness about the condition. Ms. Rambiki was one of them.
Since her treatment, she has become an advocate for fistula survivors, helping multiple women receive repairs. At this year’s event, she helped a 33-year-old friend receive treatment.
She says she still thinks back to the fateful day that she learned there was hope – and help – for women with obstetric fistula.
“That morning when my mum went to draw water saved my life,” she said.
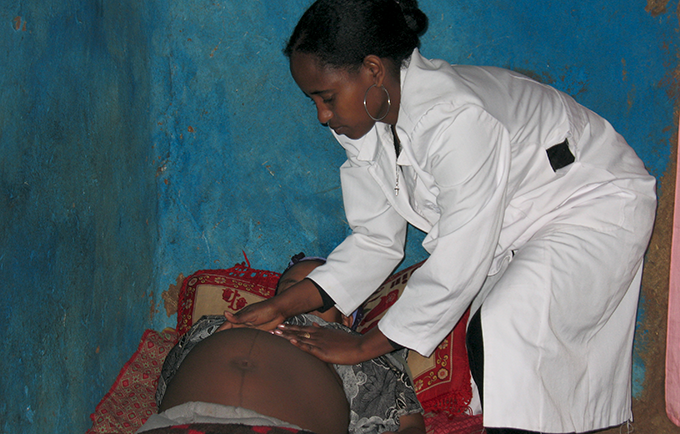
JIMMA, Ethiopia – After her wedding at age 20 in the Seka District of Ethiopia, Birkisa Aba Nega became pregnant. Then again, and again. Four of the five children she delivered died, and she was left with a debilitating childbirth injury – an obstetric fistula.
Pregnancy can be a dangerous time, and for women with ill health, malnutrition or underage pregnancy, the risks are even higher.
Read MoreJIMMA, Ethiopia – After her wedding at age 20 in the Seka District of Ethiopia, Birkisa Aba Nega became pregnant. Then again, and again. Four of the five children she delivered died, and she was left with a debilitating childbirth injury – an obstetric fistula.
Pregnancy can be a dangerous time, and for women with ill health, malnutrition or underage pregnancy, the risks are even higher.
One of the most serious complications a woman can experience in childbirth is prolonged, obstructed labour. Women who survive this condition can develop an obstetric fistula, a hole in the birth canal that leads to chronic medical problems, including pain and infection, as well as incontinence.

This misfortune is often compounded. Women who develop obstetric fistula typically also deliver a stillborn baby. And the stigma of chronic incontinence can cause women to be isolated, even shunned.
Obstetric fistula affects the most vulnerable, marginalized women – those without access to quality obstetric care. Ms. Aba Nega was one of those women. She never received antenatal services, and she delivered at home, without skilled care, for her first four pregnancies.
During her last pregnancy, she was in labour for a day and a night before an ambulance was summoned. She was taken to a health centre then transferred to a hospital, but it was too late. She lost the baby.
By the time she had returned home, she began to show signs of developing an obstetric fistula. As the condition worsened, Ms. Aba Nega’s husband began to avoid her.
She stayed home, isolated from her community, for more than a year.

These circumstances are all too common. According to a 2016 national survey, only 62 per cent of women in Ethiopia receive antenatal care, and only 28 per cent of births are attended by a skilled health provider at a health facility. A 2013 study by USAID estimated that 36,000 to 39,000 women in Ethiopia are living with obstetric fistula, and that 3,300 to 3,750 new cases occur every year.
Three years ago, the Government of Ethiopia launched a campaign to eliminate obstetric fistula by 2020. UNFPA is supporting this effort by helping to identify fistula survivors and supporting surgical repairs at hospitals in Assela, Gondar and Jimma.
UNFPA’s contribution includes training mid-level health professionals and community health workers on the prevention and diagnosis of fistula, and supplying equipment to facilitate prevention and repair efforts.
In the year after she developed the fistula, Ms. Aba Nega’s husband consulted many traditional healers, to no avail. Finally, he took her to a local health centre, which referred her to Jimma University Medical Centre.
At Jimma University, training in obstetric fistula care has been integrated into the teaching programme. Mid-level health professionals also learn to address fistula – and related conditions, such as uterine prolapse – through an in-service training programme.
Slowly, progress is being made.
Local-level health workers now identify fistula survivors and refer them to UNFPA-supported fistula repair centres.
In addition, Healing Hands of Joy, a partner in the UNFPA-led Campaign to End Fistula, is training survivors like Ms. Aba Nega to raise awareness of fistula prevention and treatment in their communities.
These efforts are paying off. More and more fistula patients are seeking help.
As for Ms. Aba Nega, she has received a surgical repair and is looking forward to helping other women do the same.
“I am very happy,” she said. “I will go back home to my husband and child. I will also inform those living with this problem in our locality to go and get treatment, like me.”
– Abraham Gelaw

SANA’A, Yemen – Shaima, 20, has experienced more than her share of suffering. Displaced by conflict, she was married off at 14, then endured pregnancy after pregnancy before her body was ready. She developed devastating complications in childbirth, including an obstetric fistula – a traumatic injury that can have lifelong consequences.
Read MoreSANA’A, Yemen – Shaima, 20, has experienced more than her share of suffering. Displaced by conflict, she was married off at 14, then endured pregnancy after pregnancy before her body was ready. She developed devastating complications in childbirth, including an obstetric fistula – a traumatic injury that can have lifelong consequences.
On Wednesday, the world will observe the International Day to End Obstetric Fistula, which calls for action to end the marginalization and inequality that perpetuate this preventable injury.

An obstetric fistula is a hole in the birth canal caused by a prolonged, obstructed labour. Left untreated, it can cause incontinence, infections, pain and a host of other problems – including social isolation, stigma and depression.
Girls who are pregnant too early, such as child brides, are especially vulnerable to this affliction, as are women who are malnourished. Malnutrition and recourse to child marriage are both on the rise in Yemen, where grinding conflict has uprooted communities, increased extreme poverty and caused the health system to collapse.
After the conflict forced Shaima’s family to flee from Sa’ada to the capital city, Sana’a, her impoverished parents married her off.
“In our community, girls are married off at a young age, like 9 or 10,” Shaima told UNFPA. “For me, I was 14 and it was considered late. I did not have a choice but to marry the first one who offered to take me. So, I wedded a widower.”
Her husband was in his 30s. Shaima was pregnant by the time she was 15, but she suffered a miscarriage.
She quickly became pregnant again, but her husband could not afford to send her to a hospital during childbirth. A neighbour helped her deliver at home, but the process was prolonged and excruciating. She developed an obstetric fistula.
And then she became pregnant once more. Again, she delivered at home. The condition worsened, as did her pain.

Shaima is not alone.
More than 2 million women in sub-Saharan Africa, Asia, the Arab region, and Latin America and the Caribbean are estimated to be living with fistula, and some 50,000 to 100,000 new cases develop annually. Yet the condition is almost entirely preventable with access to emergency obstetric care – in particular, Caesarean section.
UNFPA works around the world to help expand access to sexual and reproductive health care, including emergency obstetric care. UNFPA also supports surgical repairs for fistula survivors, and helps reintegrate survivors back into the community.
In Yemen, UNFPA has supported the establishment of two fistula units, including one at Al Thawara Hospital in Sana’a, where 28 fistula surgeries were successfully treated, free of charge, in recent months.
And in the south, 90 percent of fistula surgeries were undertaken with support from UNFPA. UNFPA has also created and strengthened a network of community volunteers, midwives, reproductive health workers and fistula experts from most of the governorates to help fistula survivors receive the services they need.

Shaima was one of these women.
After enduring months of pain, her family was finally able to send her to a local hospital. From there, she was referred to Al Thawara Hospital, where she successfully underwent fistula repair surgery.
“Now my pain is gone. I feel as if I am reborn," she said.
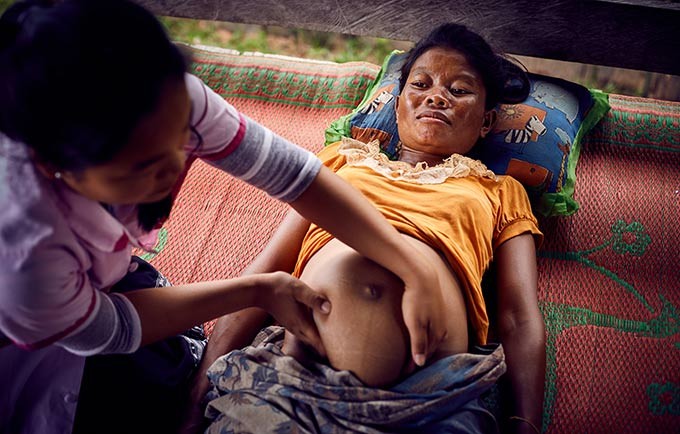
THAPANGTHONG, Lao People’s Democratic Republic – “Just lie still and relax. Breathe slowly,” midwife Khoun Keobouttavong told Out, 30. Out was laying on the floor of her small stilt house in the southern Thapangthong District of the Lao People’s Democratic Republic.
Ms. Keobouttavong pressed a fetal stethoscope into Out’s belly. Out was about six months pregnant.
“The heart is beating well,” she told Out, smiling.
Read MoreTHAPANGTHONG, Lao People’s Democratic Republic – “Just lie still and relax. Breathe slowly,” midwife Khoun Keobouttavong told Out, 30. Out was laying on the floor of her small stilt house in the southern Thapangthong District of the Lao People’s Democratic Republic.
Ms. Keobouttavong pressed a fetal stethoscope into Out’s belly. Out was about six months pregnant.
“The heart is beating well,” she told Out, smiling.
Ms. Keobouttavong is the only midwife covering the district, which includes eight villages and hundreds of residents.

Though she has a small clinic, she spends much of her time making house calls – when road conditions allow.
“For women who live in the main village, they can visit the clinic, but for those outside, there are obstacles,” she explained. “The roads are not good.”
There are also widespread misconceptions about the care she provides.
“There is a perception that antenatal care is not essential,” she said. “The previous generation gave birth at home, most often with the help of a traditional midwife [without professional training]. So sometimes they simply do not come.”
This makes it difficult to achieve one of her primary goals: reducing maternal mortality among the rural women here.
According to the most recent UN data, out of every 100,000 live births in the country, 197 women die of pregnancy-related causes – much higher than the regional average. Only about 40 per cent of births are attended by a skilled health professional, like a midwife or doctor.

There are now some 1,700 trained midwives working across the rural parts country, part of a 2012 government initiative to improve maternal health. UNFPA has supported these efforts, helping to develop a midwifery curriculum, training midwifery instructors and equipping midwifery schools.
Still, these midwives face a range of challenges – not only poor roads, but communication barriers as well. The country has dozens of ethnic groups, each with their own language and customs.
Grinding poverty also limits rural women’s access to care.
“They need to tend to rice crops and take care of children,” Ms. Keobouttavong said, explaining that many women do not have the time or resources to seek health care.
Out had to squeeze her check-up into a busy day of farm work. Afterward, she returned to the rice fields, and also cared for her two young children.
She told UNFPA that, to meet the family’s needs, she also forages for food every day. “I catch fish or frogs to eat or cut some bamboo, as we do not have money to buy food,” she said.

Khamkong, 21, is seven months pregnant. Like Out, she is a rice farmer.
She is aware pregnancies can be deadly, but comforted knowing that skilled care is available.
“I do feel very nervous because it is my first baby, and in the village where I am from, one woman died,” she told UNFPA. “I feel good having the midwife close by. I know she will take good care of me.”
The government is also looking to improve women’s health by increasing access to family planning.
Contraceptives reduce the incidence of dangerous pregnancy-related complications. Family planning also empowers women to stay in the classroom and workforce, helping them break the cycle of poverty.
“Family planning has a far-reaching social and economic impact,” said UNFPA’s representative in Lao PDR, Frederika Meijer.

UNFPA has supported the country’s family planning efforts since 1995, including by training health workers to provide contraceptive counselling and services. UNFPA has often been the sole provider of contraceptives to the government health system.
UNFPA is also working to keep midwifery care up-to-date. Last year, UNFPA released a mobile phone app for midwives, which contains the most recent clinical guidance as well as instructional videos.
For her part, Ms. Keobouttavong says that, although she is sometimes overwhelmed with the workload, she happy to see an increase in women seeking her services.
She hopes to set an example for the next generation.
She, too, grew up in the area, she explained. She was the only woman in her village to ever graduate from secondary school.
“I have some girls who want to talk to me about my education and some of the parents see that maybe it’s good for their daughters to stay in school. People see what I have done and so they have begun to think, maybe I can do that too,” she said.
– Ruth Carr

KOLLA TEMBEIN, Ethiopia – Not long ago, the sight of a 10-year-old bride was a common occurrence in Ethiopia’s Kolla Tembein District, said Daniel Hagos, the district’s chief administrator. But the community’s women and girls are mobilizing to change things – and they are seeing enormous success.
“We are getting remarkable results in the fight against child marriage,” said Atsede Girmay, one of the volunteers in this effort.
Read MoreKOLLA TEMBEIN, Ethiopia – Not long ago, the sight of a 10-year-old bride was a common occurrence in Ethiopia’s Kolla Tembein District, said Daniel Hagos, the district’s chief administrator. But the community’s women and girls are mobilizing to change things – and they are seeing enormous success.
“We are getting remarkable results in the fight against child marriage,” said Atsede Girmay, one of the volunteers in this effort.
Child marriage is a global phenomenon, one that leaves girls vulnerable to abuse and health problems, including potentially deadly pregnancy complications .
In Kolla Tembein, the practice is deep-rooted, with many people believing that girls should marry while they are young and “pure”.
But three years ago, community groups began working with UNFPA to raise awareness of the harms of child marriage. Then through the UNFPA-UNICEF Global Programme to Accelerate Action to End Child Marriage, efforts were targeted towards three localities in the district where child marriage was most prevalent.
Central to their approach is empowering women and girls to stand up and take action themselves.

The programme works with women’s volunteer networks called Women’s Development Groups. The volunteers received information about the consequences of child marriage, as well as related issues such as gender equality, the importance of ending female genital mutilation (FGM), and the benefits of maternal health care.
Some volunteers, like Ms. Atsede, were selected to become a facilitator for the broader community. Ms. Atsede received a teaching manual and training to engage people on the subject of child marriage.
Now, every Sunday, she meets with 35 adolescent girls and their families to discuss the issue.
“We teach how child marriage isolates a girl, how it will force her to drop out of school, and how it will end in serious health hazards such as obstetric fistula,” Ms. Atsede explained.
Because girls who leave school are more likely to be married off, and because many child brides are forced to drop out, the Women’s Development Groups also work closely with the local schools. If a girl drops out, the volunteers speak with her family to convince them of the importance of education over early marriage. If necessary, they refer cases of child marriage to local authorities.
In schools, girls’ clubs are also helping to end child marriage. The clubs meet every two weeks with a specially trained mentor, who explains the harms of child marriage.
The girls also receive other information, including the basics of sexual and reproductive health and how to prevent sexually transmitted infections. They also gain life skills such as financial literacy skills.
The idea is to empower girls to not only reject child marriage, but to minimize their vulnerability by improving their prospects for the future.

Merhawit Mezgebe, 18, is a 10th grader, and has been attending this programme for the past two years. Like other girls in the club, she has opened a savings account and is eager to plan for her future.
“I want to use my savings to finance my college studies without bothering my parents,” she said, smiling.
The girls are also helping to stamp out child marriage in their communities, she added.
When members of the club hear about possible child marriages taking place, they report it back to their mentor, who works with authorities to take action.
In 2014, Ethiopia committed to end child marriage by 2025.
But Mr. Daniel says Kolla Tembein is on track to meet this goal even earlier. “My district will attain the commitment the country made to end child marriage before the set target date,” he said.
In the three high-risk localities where the programme is being implemented, some 1,200 unmarried girls were reached through school programmes like the girls’ clubs. Community outreach efforts engaged another 1,200 girls who were already married.
Thanks to such efforts, Mr. Daniel says, there have not been any cases of child marriage reported in those localities in the past last three years, and the dropout rate among female students has fallen to almost zero.
The programme now is set to expand to the rest of the district.
– Abraham Gelaw