News & Updates
Obstetric fistula stories and announcements
Obstetric fistula stories and announcements
Obstetric fistula is a preventable and treatable childbirth injury, but an estimated half a million women and girls globally continue to suffer its devastating effects. This short animated video highlights the painful realities of fistula and calls for urgent action to prevent and treat this neglected condition. Watch the video to understand why we must act now to End Fistula.
Watch the videoObstetric fistula is a preventable and treatable childbirth injury, but an estimated half a million women and girls globally continue to suffer its devastating effects. This short animated video highlights the painful realities of fistula and calls for urgent action to prevent and treat this neglected condition. Watch the video to understand why we must act now to End Fistula.
Watch as Dr. Mohan Chandra Regmi from Nepal speaks about obstetric fistula - a devastating condition that can have life-altering effects on a woman's physical and emotional well-being.
Watch the videoWatch as Dr. Mohan Chandra Regmi from Nepal speaks about obstetric fistula - a devastating condition that can have life-altering effects on a woman's physical and emotional well-being.
In the heart of Islamabad, Pakistan, a young woman named Sobia faced an unimaginable ordeal: obstetric fistula. This debilitating condition left her ostracized and hopeless, but her spirit remained unbroken. Join us as we share Sobia's incredible journey of survival, resilience, and the unwavering hope that led her to reclaim her life.
Watch the videoIn the heart of Islamabad, Pakistan, a young woman named Sobia faced an unimaginable ordeal: obstetric fistula. This debilitating condition left her ostracized and hopeless, but her spirit remained unbroken. Join us as we share Sobia's incredible journey of survival, resilience, and the unwavering hope that led her to reclaim her life.

BUJUMBURA, Burundi – “During my contractions, my mother-in-law and my own mother refused to let me go to the health centre to give birth,” Gloriose Mbonimpa told UNFPA, the United Nations sexual and reproductive health agency. “I felt death was approaching.”
Read MoreBUJUMBURA, Burundi – “During my contractions, my mother-in-law and my own mother refused to let me go to the health centre to give birth,” Gloriose Mbonimpa told UNFPA, the United Nations sexual and reproductive health agency. “I felt death was approaching.”
Isolated from the medical care she needed, Ms. Mbonimpa shouted to her neighbours for help. They tried to take her to the local medical centre, but it was too late; she gave birth on the way, delivering a stillborn baby and suffering an obstetric fistula in the process.
Obstetric fistulas are childbirth injuries that result mainly from prolonged, obstructed labour. Around the world, these injuries affect nearly half a million women and girls – especially those lacking access to timely, high-quality medical support. In Burundi, where Ms. Mbonimpa lives, it is estimated that women and girls sustain up to 750 new fistula injuries every year.
The consequences can be devastating. Fistula survivors are often forced to deal with traumatic physical ailments, including incontinence, social ostracism and extreme poverty.
“Women in the maternity ward asked that I be isolated because I wet the bed. In addition to the pain of having lost my baby, I didn’t understand what was happening to me,” Donavine Ndayikengurukiye, another fistula survivor, told UNFPA.
Meanwhile, Ms. Mbonimpa’s husband abandoned her for four years following her injury. Ashamed, she also lied to health-care providers about her condition. “I was giving off unbearable odours,” she said. “No one deserves to experience this.”
Once ashamed, now an advocate
Fistulas can be fixed. Yet research shows many survivors are unaware that surgery can help heal their injuries.
Initially, Ms. Ndayikengurukiye was one of them. But “learning that I had the chance to recover was the best news of my life,” she told UNFPA.
In Burundi, just one health facility – the Urumuri Centre in the country’s capital, Bujumbura – is equipped to handle fistula cases. Between 2010 and 2023, approximately 3,000 women underwent repair surgeries there.
Ms. Mbonimpa was one of them. In 2022, she sought treatment at the centre during a UNFPA-supported campaign that offered fistula survivors access to free health care.
For two decades she had lived in isolation, humiliated by her condition. But since recovering she has made a promise: To dedicate the next two to raising awareness about obstetric fistula so that no other woman or girl in her community has to suffer the same experience.
Ending fistula for ever and for all
While surgery offers survivors the opportunity to heal, the best way to end the harm fistulas cause women and girls is to prevent them from occurring in the first place.
The prevalence of obstetric fistula follows patterns of inequality: Almost absent from high-income countries, the condition mainly affects women and girls in the Arab States region, Asia, Latin America and the Caribbean and sub-Saharan Africa.
“Obstetric fistula is a tragic result of our failure to protect the reproductive rights of the most vulnerable and excluded women and girls,” said UNFPA Executive Director Dr. Natalia Kanem.
Adolescent girls can be especially vulnerable to the injury, as their pelvises may not have developed sufficiently for childbearing, putting them at risk of obstructed labour.
“I think I got this [fistula] because I gave birth when I was very young,” Ms. Ndayikengurukiye told UNFPA.
Twenty-three years old and now fistula-free, Ms. Ndayikengurukiye is mother to a little girl whose birth took place one year following her recovery. Since then, she and her husband have embraced family planning.
“My husband and I chose family planning so that my body could rest from the risk of having another obstetric fistula, and to wait for our little girl to grow up a little bit,” she said.
This is the story of Adelia, a fistula survivor whose journey to healing highlights the devastating impact of this preventable childbirth injury. Through Adelia's experience, we witness the transformative power of timely medical intervention and the importance of supporting initiatives that ensure accessible and quality maternal healthcare to prevent and treat fistula.
Watch the videoThis is the story of Adelia, a fistula survivor whose journey to healing highlights the devastating impact of this preventable childbirth injury. Through Adelia's experience, we witness the transformative power of timely medical intervention and the importance of supporting initiatives that ensure accessible and quality maternal healthcare to prevent and treat fistula.

CONAKRY, Guinea – “It happened at the hospital. I realized I was leaking urine,” fistula survivor Kadiatou Bah told UNFPA, the United Nations sexual and reproductive health agency.
Read MoreCONAKRY, Guinea – “It happened at the hospital. I realized I was leaking urine,” fistula survivor Kadiatou Bah told UNFPA, the United Nations sexual and reproductive health agency.
Ms. Bah first fell pregnant more than four decades ago, when she was 17. With few health centres on hand in her mountainous village in Labé, Guinea, she’d had little chance to avail herself of services during her pregnancy; nor had she planned to give birth at a health facility.
But her plans changed after two days of labour. “When we wanted to go to the health centre, I gave birth on the way,” she said. “The child was already dead.”
Though she didn’t realize it at the time, Ms. Bah had suffered an obstetric fistula: A devastating childbirth injury that carries life-threatening risks for women and their pregnancies. About nine in ten women who develop obstetric fistula suffer stillbirths; meanwhile, research shows obstructed labour drives 6 per cent of maternal deaths.
Fistula’s effects are also severe for survivors; many encounter incontinence, mental and physical ailments and societal ostracization. Ms. Bah’s disability drove a wedge between her and her husband, who offered her little support.
“I could no longer show myself in public,” she said. “People avoided me; I suffered a lot.”
A road to recovery
Half a million women and girls across the Arab States, Asia, Latin America and the Caribbean, and sub-Saharan Africa are estimated to be survivors of obstetric fistula. Many are girls and young women who, like Ms. Bah, were married as children and may have become pregnant before their bodies were developmentally ready.
According to 2018 data, about 124,000 women in Guinea are affected by obstetric fistula – more than 4 per cent of women of childbearing age in the country.
Despite its prevalence, survivors of obstetric fistula remain subject to extreme levels of stigma. “Among the complications linked to pregnancy, obstetric fistula is one of the most serious, as it also causes social exclusion,” said Dr. Sékou Diallo, a gynaecologist in Mamou.
According to experts, caring for fistula survivors requires addressing their medical, psychosocial and socioeconomic needs. Most fistulas can be repaired via surgery, although this can be difficult to access given the global lack in surgeons trained to provide this care. In Guinea, for example, only one hospital in the country’s northeast regularly offers fistula repair surgeries.
Despite these challenges, more than 500 women were able to obtain free fistula care between 2018 and 2023.

Fistula-free
Ms. Bah had lived with obstetric fistula for almost 20 years before her first repair surgery. “I underwent a first operation, then [a second], but I was still losing urine,” she said.
Following a third surgery in 2019, however, she was able to make a full recovery.
With UNFPA’s support, the Government of Guinea has developed a national strategy to combat obstetric fistula, creating fistula management units across seven regions of the country. Within these units, teams of surgeons, nurses and anaesthetists are trained to offer fistula repair surgeries to help women like Ms. Bah heal.
"Obstetric fistula is a tragic result of our failure to protect the reproductive rights of the most vulnerable and excluded women and girls,” said UNFPA Executive Director Dr. Natalia Kanem.
“By addressing deep-rooted inequalities, reaching those furthest behind, and investing in universal access to timely, high-quality maternal health services, we can and must end fistula once and for all.”
This is part of a series of stories illustrating progress made since the 1994 International Conference on Population and Development, which committed to ensure gender equality and the right to sexual and reproductive health for all. Find out more.

TAMBACOUNDA REGION, Senegal – “After giving birth, I developed a fistula and my life was turned upside down,” said Khady* at her home in the village of Koumpentoum, deep in Senegal’s southern Tambacounda region.
“For almost 40 years, my faeces mixed with my urine and was constantly leaking. I lost friends and was no longer invited to christenings or other ceremonies.”
Read MoreTAMBACOUNDA REGION, Senegal – “After giving birth, I developed a fistula and my life was turned upside down,” said Khady* at her home in the village of Koumpentoum, deep in Senegal’s southern Tambacounda region.
“For almost 40 years, my faeces mixed with my urine and was constantly leaking. I lost friends and was no longer invited to christenings or other ceremonies.”
Obstetric fistula is a tear to the birth canal, bladder or rectum that causes severe physical and psychological pain. It is typically caused by prolonged or obstructed labour; girls who give birth at too young an age, when their bodies are not yet ready, are especially vulnerable to this traumatic birth injury.
Although it can be relatively easily avoided with the assistance of trained midwives (and in fact it is almost nonexistent in communities with access to basic emergency obstetric care) or repaired by obstetric surgeons, half a million women and girls around the world are estimated to be living with fistula, with tens of thousands of new cases developing every year.
In addition to the discomfort and subsequent infections the condition can lead to, women and girls with obstetric fistula are also often stigmatized and abandoned by their families, partners and communities. Unable to work, the slide into poverty, isolation and extreme vulnerability can be all-too swift.

Breaking the silence
UNFPA, the UN sexual and reproductive health agency, and local partners are raising awareness about obstetric fistula among rural communities and securing the funds needed to perform surgical repairs in even the most remote areas. Advocacy efforts and group discussions bring together women from across generations, helping them to learn and recognize the signs of obstetric fistula.
Although exact data are challenging to come by, the highest prevalence of obstetric fistula in Senegal has been reported in the Tambacounda region, where access to health care is scarce and many give birth unassisted at home or with only limited support.
A midwife who joined the community discussion explained how the debilitating condition is linked to early marriages and pregnancies, home deliveries and inadequate access to skilled health workers. These same factors all also lead to delays in treatment.
Adama* said that a neighbour had been suffering from fistula in secret, ashamed to tell anyone or ask for help. The neighbour was stigmatized by older members of the community and rejected by her family.
“The grandmothers said she was cursed…Then her husband abandoned her. We didn't see her any more.”
But after attending an awareness-raising session, Adama said, “From the chat we had, I realized that she had a fistula.” She and her neighbours then understood what was really going on and offered their support.

Working together to eradicate obstetric fistula
Since 2018, UNFPA with the support of the Government of Canada has provided surgical care for more than 300 women in the southern Kolda and Sédhiou regions, as well as carrying out awareness-raising sessions and establishing a reception centre with three bedrooms. Each patient was consistently monitored and, once they had recovered, participated in capacity-building sessions on personal finance and livelihoods skills.
For 20 years, UNFPA has led the global Campaign to End Fistula by 2030 through advocacy, prevention, treatment and social reintegration of survivors.
Prevention strategies include family planning among vulnerable communities to avoid unintended pregnancies, child marriage and early pregnancy among adolescents. Meanwhile, advocates are encouraging antenatal consultations, childbirth assisted by qualified personnel in an equipped maternity hospital rather than at home, and emergency neonatal obstetric care, including timely caesarean sections.
Beyond being a pressing public health issue, the fact that so many women and girls are at risk of developing obstetric fistula is a barrier to their human right to live with dignity and in good health.
With dedicated social support, thousands of women like Khady are gradually recovering and reintegrating back into their communities. After six cost-free repair surgeries and with consistent follow-up care, she has even managed to set up a small business selling sweets and basic groceries from her home.
“I have my life back,” she told UNFPA.
* Names changed for privacy and protection.

NKHATA BAY, Malawi – Jacqueline was just 15 when she fell in love with a boy from another village. The two eloped, initiating a customary marriage rather than a formal one. But Jacqueline kept the relationship a secret from her mother, Margaret Kumwenda, who grew worried about her daughter’s increasing distraction and frequent disappearances.
Read MoreNKHATA BAY, Malawi – Jacqueline was just 15 when she fell in love with a boy from another village. The two eloped, initiating a customary marriage rather than a formal one. But Jacqueline kept the relationship a secret from her mother, Margaret Kumwenda, who grew worried about her daughter’s increasing distraction and frequent disappearances.
When Ms. Kumwenda learned about the elopement, she was upset, even asking the police to take action against the boy. “They told me that he was still a minor, and all they could do was counsel him and Jacqueline,” she recently recalled to UNFPA, the UN sexual and reproductive health agency.
The counselling seemed to work for a time. Jacqueline, who had always been a hardworking student, applied a renewed dedication to her studies. Ms. Kumwenda hoped her daughter would finish her education before getting serious about her relationship.
But dropout rates are high for girls in Jacqueline’s remote community, which is an hour’s walk from the nearest school. Early marriage is often seen as inevitable for teenage girls, who commonly receive little information – if any – about their sexual and reproductive health and rights.
With no hope for a different future, Jacqueline, too, decided to leave school. One day, she packed up her belongings and ran away with her husband, moving to Mzimba District.
“We tried looking for her, but to no avail,” Ms. Kumwenda said.
Childbirth injury and abandonment
Jacqueline soon became pregnant and, at age 16, went into labour at a local health facility. The delivery was obstructed, prolonged and agonizing, resulting in an obstetric fistula – a traumatic childbirth injury in which a hole is torn in the birth canal. Adolescent girls, in particular, are vulnerable to obstructed labour and obstetric fistula.
Eventually Jacqueline delivered a baby girl. The baby thrived in the days following the birth, but Jacqueline did not. Like most fistula survivors, she began to leak faeces and urine, and her injuries failed to heal.
“My life was lonely as I couldn’t go out of the house because I was wetting myself,” Jacqueline later recounted to UNFPA. For months she was isolated, confined indoors by her injuries.
Then one day, her husband decided to send her away. Tragically, abandonment by a spouse or family is common among fistula survivors. Afraid of contacting Ms. Kumwenda directly, the boy sent an anonymous message through an intermediary: Your daughter is unwell and wants to come home.

Human rights at stake
The reunion was bittersweet for Ms. Kumwenda. She was relieved to have her daughter home, and overjoyed to meet her baby granddaughter. At the same time, her daughter’s condition devastated her.
“I didn’t know what to do,” said Ms. Kumwenda.
An untreated fistula can cause serious physical ailments – not only chronic incontinence but also frequent infections and possible infertility. But obstetric fistula is not simply a health issue. It is a human rights issue.
In most of the world, obstetric fistula is preventable with access to emergency obstetric care – usually a Caesarean section. Today, this condition overwhelming affects the most vulnerable women and girls: those with limited access to the comprehensive sexuality education that would enable them to prevent an adolescent pregnancy, those who experience child marriage, and those without access to a skilled birth attendant and competent emergency care during delivery.
The consequences of fistula only compound the hardships these women and girls face. They experience stigma, discrimination from communities, families and employers, and often lasting psychological harm.
A new path
But Ms. Kumwenda refused to give up. “I remembered that there was a woman in our community who always talked about a similar condition, and how she can help to get it treated,” she recalled.
The woman was a fistula ambassador for the Spotlight Initiative, a gender equality programme funded by the European Union and implemented by UNFPA and other United Nations agencies. “She agreed to come to our house the next day,” Ms. Kumwenda said.
Soon, Jacqueline was referred to the Nkhata Bay District Hospital, and from there she was scheduled for surgery at the district health office, supported by the Spotlight Initiative.
“I don’t know what could have happened if I didn’t come here,” she said at the hospital, after the repair surgery.
UNFPA and Spotlight are also working with the local community to address the root causes of obstetric fistula: the vulnerabilities of women and girls. Together with the Nkhata Bay District Council, they are empowering women and girls with knowledge about sexual and reproductive health and rights.
As for Jacqueline, she is now healed and able to think about her future – and that of her two-year-old daughter – and she has some powerful new role models. “I thank those who helped me get well again,” she said.

BISSAU, Guinea-Bissau – “I didn't know what obstetric fistula was, let alone that it could be treated,” says 33-year-old mother-of-two Maria.
Maria’s dream of expanding her family took a tragic turn in 2016. She was in eastern Guinea-Bissau, in Batafa region, when her labour pains began; but after more than 12 hours, she remained unable to deliver.
Read MoreBISSAU, Guinea-Bissau – “I didn't know what obstetric fistula was, let alone that it could be treated,” says 33-year-old mother-of-two Maria.
Maria’s dream of expanding her family took a tragic turn in 2016. She was in eastern Guinea-Bissau, in Batafa region, when her labour pains began; but after more than 12 hours, she remained unable to deliver.
Maria was evacuated to the Simão Mendes National Hospital in Guinea-Bissau’s capital, but upon her arrival three hours later, an echography revealed her baby had died in utero.
Hours later, after being discharged from the hospital, Maria felt herself leaking bodily fluids. She had suffered an obstetric fistula, a devastating injury resulting from prolonged, obstructed labour, which causes incontinence.
Around the world, half a million women and girls are estimated to be living with obstetric fistula. Despite the condition’s prevalence, many women and girls who have sustained the injury find themselves abandoned and ostracized by family and community – resulting in both physical and psychological trauma.
Sadly, this was the case for Maria. “I used to think about suicide because of the severe stigma I suffered,” Maria said. “My family completely abandoned me.”*
Creating a virtuous cycle
As fistula does not just affect bodies, but lives and minds as well, the UNFPA-led Campaign to End Fistula works with communities around the world to provide both fistula repair surgeries and psychosocial support geared towards helping women and girls reintegrate into society.
In Guinea-Bissau, UNFPA worked in partnership with the government of Guinea-Bissau to provide free fistula repair surgeries to 42 women – three of whom were offered scholarships to train as midwives at the country’s National School of Health.
“This training opportunity will be rewarding for my integration into society,” says Vitoria, who received one of the scholarships. “I hope it will be extended to more women who are victims of this terrible disease.”
The programme aims to empower survivors to rejoin communities, with the knock-on effect of fortifying Guinea-Bissau’s cadre of midwives. These providers have been singled out for their critical role in preventing the occurrence of obstetric fistula in the first place.
“To end fistula, we need to make sure that all women and girls have timely access to trained midwives and high-quality obstetric care,” UNFPA Executive Director Dr. Natalia Kanem said on the 2023 International Day to End Obstetric Fistula. “That’s why UNFPA is working to scale up the midwifery workforce and close the global gap of nearly 1 million midwives.”

A chance at fistula repair heard over the airwaves
In 2021, Maria heard a radio advertisement that changed her life. It was for the treatment of obstetric fistula, and described the condition’s symptoms as similar to those she experienced.
She had not known the name of her condition, but received a diagnosis of obstetric fistula after seeking care at the Simão Mendes National Hospital in Bissau.
Two surgeries were required to repair her injury; the second was completed in 2022.
"After the repair, my life completely changed,” Maria said. “I feel wonderful. I don't use pads anymore."
*If you are struggling with suicidal thoughts, depression, trauma or any other mental health concerns, please seek help and advice from a trusted health provider as soon as possible.
NORTH-WESTERN PROVINCE, Zambia – Around the world, half a million women and girls are thought to be living with obstetric fistula, a serious childbirth injury that can cause incontinence and result in significant medical and mental health issues. In Zambia, as of 2018, more than 33,000 women and girls had been affected.
Read MoreNORTH-WESTERN PROVINCE, Zambia – Around the world, half a million women and girls are thought to be living with obstetric fistula, a serious childbirth injury that can cause incontinence and result in significant medical and mental health issues. In Zambia, as of 2018, more than 33,000 women and girls had been affected.
For over a decade, the Government of Zambia and UNFPA have partnered to provide fistula survivors with life-transforming surgeries aimed at healing their physical and psychological wounds. Many of these procedures are conducted at fistula camps held at Zambia’s main provincial hospitals, where three or more doctors gather to perform surgeries for several days.
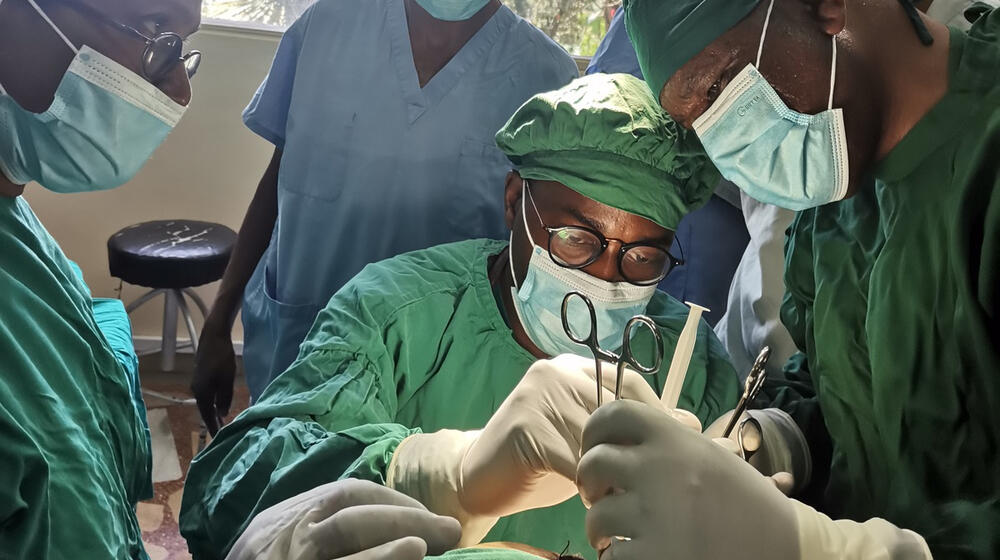
Dr. Paul Musoba is one of just eight fistula surgeons in the country. On the occasion of the International Day to End Obstetric Fistula, UNFPA sat down with Dr. Musoba, who works at the Solwezi general hospital in Zambia’s North-Western Province, to learn more about what drew him to this field of surgery, the challenges he encounters in his work and the successes that have made him proud to be a fistula surgeon. This interview has been edited and condensed.
What inspired you to become a fistula surgeon?
Early in my practice as an obstetrician and gynaecologist, I encountered many women and girls who had suffered greatly from obstetric fistula. Seeing women and girls abandoned and ostracized due to their constant leakage of urine, faeces or both was the starting point of my desire to change the narrative.
Taking inspiration and mentorship from some of Zambia’s senior fistula surgeons, I first participated in a fistula camp in 2019. I was able to observe, assist and eventually undertake fistula surgeries. It is definitely a specialized skill that requires constant practice and exposure.
It is quite fulfilling, but at the same time, challenging.
Can you talk about the scope of the problem of fistula in Zambia?
Pregnancy and childbirth should be among the happiest times in a woman’s life. Sadly, this is not the case for thousands of women and girls not only in North-Western Province, where I am located, but across Zambia at large.
At the Solwezi general hospital, I often encounter women and girls who have developed obstetric fistula, some of whom have lived with the condition for years.
How do you approach meeting the specific needs of fistula patients?
My journey begins with me getting to understand their situation. The trauma suffered by many of my clients during delivery is heartbreaking, as it goes beyond the physical. I focus throughout not only on healing their physical wounds, but also supporting their emotional and psychological healing.
During fistula camps, my surgical work typically begins at 7:30 a.m. and ends at 6 p.m., with 15-minute intervals in the operating theatre between clients. This maximizes on time against high demand.
The process concludes with a hospital discharge of a happy, “dry” and “continent” client. It makes me proud to be a fistula surgeon.
What are some of the challenges you face while working to support women and girls affected by fistula?
Every year, I repair an average of ten fistula clients, at either the Solwezi general hospital or during fistula camps at other hospitals. However, I know there are many other women suffering with fistula who are not able to access treatment due to lack of information or challenges in accessing health care.
Getting to expectant mothers, as well those suffering from fistula in their communities, is therefore one of the biggest challenges I face. Many women in North-Western Province live in remote areas located far from health facilities, often resulting in home deliveries – a key risk factor for obstetric fistula in the event of obstructed labour.
Additionally, for many fistula survivors, societal stigma still remains a major issue. Successful reintegration is a key priority post-surgery.
Can you share a story from your work with fistula patients that has stuck with you?
My recent encounter with an 18-year-old fistula survivor stands out to me. She developed obstetric fistula due to obstructed labour and delayed access to emergency health care, and lost her baby.
For two years she lived with fistula and could not continue with her education. But with the help of community health workers, she was able to access surgical care, and I successfully repaired her fistula.
Throughout this process, she was very jovial and optimistic; her confidence put pressure on the team. I personally made a follow-up visit four months after her operation, and the girl we had discharged had an even brighter smile.
She told me: “Dr Musoba, thanks to you, I have now gone back to school and am looking forward to completing my education!”