News & Updates
Obstetric fistula stories and announcements
Obstetric fistula stories and announcements

MOCUBA, ZAMBEZIA PROVINCE, Mozambique – Beatriz Sebastião suffered in silence. She had no friends in the neighborhood or at school. When she went to church, she sat alone. When she went to the river, other women mocked her before leaving to bathe elsewhere.
Read MoreMOCUBA, ZAMBEZIA PROVINCE, Mozambique – Beatriz Sebastião suffered in silence. She had no friends in the neighborhood or at school. When she went to church, she sat alone. When she went to the river, other women mocked her before leaving to bathe elsewhere.
She had become pregnant at 15 and because she lived far from the hospital, planned to give birth at home. After three days of labour, her parents had to raise money to rent a motorcycle to take her to the hospital, where she delivered a stillborn child. She developed an obstetric fistula, and when she became pregnant again, that child, too, was stillborn. But the fistula caused urine to leak, and the resulting smell isolated her from nearly everyone for the next six years.
A treatable, preventable condition
Obstetric fistula is a hole between the birth canal and bladder or rectum, which can cause incontinence, leading to social ostracization and attendant psychological issues like depression. The treatable and largely preventable condition is the result of prolonged, obstructed labour with no access to skilled care, often resulting in stillbirth. Girls whose bodies are too young to deliver a baby are particularly vulnerable.
Every year, there are an estimated 2,500 reported fistula cases in Mozambique, of the 50,000 to 100,000 cases globally. Since 2018, in partnership with the Government of Mozambique, UNFPA has supported the repair of more than 2,300 fistulas, recruited 28 fistula surgeons, expanded a real-time monitoring system of cases to 25 health facilities, and educated thousands of people about the causes and consequences of the condition.
A life transformed
Ms. Sebastião, now 28, had once sung gospel and six years after developing the fistula, received a fateful invitation to perform at a youth meeting. Encouraged by an uncle, she went, “but as always, I was discriminated against. I was humiliated. People talked. Because of the looks, I stayed there shrunken.” She stayed alone in a tent because no one would share space with her.

Then the youth coordinator, who also worked at a hospital, sought her out when she skipped practice, claiming illness. Finally, she admitted she had “a disease that made me pee involuntarily,” which is when she learned that what she had could be cured through surgery.
Ms. Sebastião was one of the rare fistula survivors whose family and husband did not abandon her. With their support, she had the operation and, for the first time in years, awoke without having wet the bed. “I don’t know how to express what was in my heart,” she recalled. “I had emotions I don’t know how to describe.”
She was no longer the person others fled from. She could wear skirts again, instead of covering herself with multiple layers of cloth. She started a small grocery business, something unthinkable before, and became an activist, holding chats with women in various communities to discuss fistula. She learned “to love that Beatriz from the past again,” she said. “When I had the disease, I was nothing. Now, I am capable of everything, able to fight for my well-being and raise my self-esteem.”
The contagious joy of a woman with a repaired fistula
Albertina Luis is a radio journalist and activist in Mocuba District. When her activism focused on domestic violence, she would meet women hiding behind their houses or in the cassava trees – not from abusive husbands but because they had obstetric fistulas. Ms. Luis underwent reproductive sexual health training and learned more.

Now, through regular broadcasts, she reduces shame and stigma surrounding obstetric fistula and lets women know how to prevent it, including avoiding forced, premature marriage and unintended pregnancy, and where to seek medical treatment. “Dignity means being valued,” Ms. Luis, 50, said. “The greatest wealth is health. In addition to being a right, it is power. I am freeing women who have lost their dignity for a long time.”
Dr. Armando Rafael, a fistula surgeon at Mocuba Rural Hospital, who operated on Ms. Sebastião, finds his work rewarding, knowing the suffering and marginalization patients have endured. “The contagious joy of a woman when her fistula is repaired is incomparable,” he said.
During Ms. Sebastião’s long exile, women at the river taunted her with the cruel nickname “Lake Bethesda,” a reference to the Bible's Pool of Bethesda that never ran dry. For her, the name takes on a different significance now: in Biblical lore, the pool was a place where miracles happened and people were healed.


The most vulnerable women
Under the shadow of war
Support needed

BOUAKÉ, Côte d'Ivoire
Read MoreBOUAKÉ, Côte d'Ivoire – When Blandine was pregnant, she didn't go to the hospital for regular prenatal check-ups. On the day she gave birth, she delayed in going to the health centre. Her doctor told her that's why the birth had complications which resulted in her developing obstetric fistula.
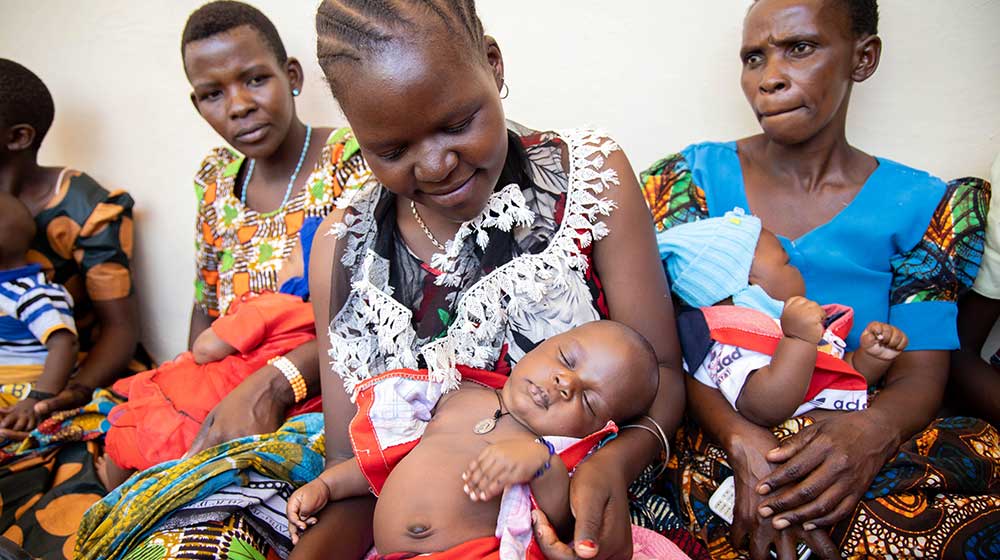
Sahar survived a painful experience during the birth of her daughter, Sondos. She was then determined to be part of the solution so other women in her community don't experience the same pain.
Two thirds of all reproductive health facilities in Yemen stopped working since the start of the war. This leaves millions of Yemeni women vulnerable to increased rates of maternal mortality and morbidity.
Watch the videoSahar survived a painful experience during the birth of her daughter, Sondos. She was then determined to be part of the solution so other women in her community don't experience the same pain.
Two thirds of all reproductive health facilities in Yemen stopped working since the start of the war. This leaves millions of Yemeni women vulnerable to increased rates of maternal mortality and morbidity.
Read more about Sahar and women's lives in Yemen: https://bit.ly/2EbSD2I
Follow #WomenOnTheFrontline and join our call to prioritize women's needs in humanitarian response.

ISLAMABAD, Pakistan – “Helping women suffering fistula is my mission in life," Razia Shamshad said about the maternal injury from childbirth that she thought would ruin her life. “No woman deserves to live in misery, especially when it is treatable.”
Read MoreISLAMABAD, Pakistan – “Helping women suffering fistula is my mission in life," Razia Shamshad said about the maternal injury from childbirth that she thought would ruin her life. “No woman deserves to live in misery, especially when it is treatable.”
Ms. Shamshad, 29, was born in a small village in southern Punjab. Her family did not want her to go to school, so she had only received an informal religious education by age 13, when she was married off. Ms. Shamshad was already expecting her first baby within a few weeks of her wedding. Then, when she was six months pregnant, her husband died in a road accident.
Unable to afford proper medical care, Ms. Shamshad was assisted by an unskilled traditional birth attendant who was unable to manage complications. When Ms. Shamshad suffered an obstructed labour, the birth attendant did not summon medical help. Ms. Shamshad was in agony for four days, an ordeal that could have killed her.
In the end, her daughter was stillborn, and Ms. Shamshad suffered serious damage. She developed an obstetric fistula, a hole in the birth canal. Fistula leaves women leaking urine, faeces or both, and often leads to chronic medical problems.
The condition is preventable with timely access to quality medical care, such as Caesarean section. Tragically, it persists among the most marginalized women, with pregnant adolescents and undernourished women facing particularly high risks. And its sufferers are further marginalized, often facing ostracism and discrimination.
"People would either avoid me or just make fun of me," she said. "I never felt clean."
But Ms. Shamshad was able to put her life back together. Her relatives learned about free treatment available at the Koohi Goth Women’s Hospital, which specializes in treating fistula and other conditions related to reproductive health. Two years after her ordeal, her family paid for her to travel to Karachi for care.
Ms. Shamshad’s condition was complex, and required multiple surgeries between 2010 to 2016. Even so, she has been able to regain her life.
“Her determination was exceptional. She was resilient and strong and was able to pull through the difficult process successfully,” said Dr. Sajjad Ahmed, who was trained by UNFPA to perform fistula repair surgeries.
Ms. Shamshad went on to meet her current husband. They adopted a little girl. And though she was not expected to be able to get pregnant again, she surprised everyone by conceiving. With regular prenatal care and a C-section, she had a healthy baby girl.
In many ways, Ms. Shamshad was lucky. The story is very different for many fistula survivors in Pakistan, who are unaware that there is treatment available.
And many more women and girls are at risk. Access to reproductive health services remains a challenge for women in Pakistan. Only an estimated 52 per cent of women give birth with the help of a skilled attendant, leaving them vulnerable to complications like prolonged, obstructed labour.
In partnership with the Pakistan National Forum on Women's Health, UNFPA has established treatment centres for fistula patients across the country. UNFPA also supports campaigns to raise awareness about the importance of skilled obstetric care and ending the stigmatization of women with fistula.
UNFPA leads the global Campaign to End Fistula. Since 2003, UNFPA has helped perform over 105,000 surgical fistula repairs in more than 55 countries in Africa, Asia, the Middle East and Latin America.
Today, Ms. Shamshad lives with her family in Karachi. She volunteers at the same hospital where she received the treatment that turned her life around. Ms. Shamshad helps new patients recover after their own treatment.
“I believe life experiences shape us into the people we need to become," she told UNFPA. "My experiences have given me the courage and drive to help women who have lost all hope because of fistula.”
Ms. Shamshad recently represented the hospital at the Nairobi Summit on ICPD25 in November 2019. She used her story to inform and motivate other women, to whom she has proven to be a source of encouragement.
"Never give up hope," she told them.

LILONGWE, Malawi
Read MoreLILONGWE, Malawi – Monica Kaleso loved to go to school. She studied hard and never missed class. Her dream of becoming a medical doctor was on course until 2013, when, at the age of 17, she began a relationship with a man from the same village of Kadammanja.
Later that year, Ms. Kaleso discovered she was pregnant. Her world crumbled.
Her boyfriend refused to take any responsibility. Ms. Kaleso was devastated. She eventually dropped out of school.
After going into labour, Ms. Kawelo struggled to find reliable transportation for the bumpy journey to the hospital. When she finally did arrive, she was unable to get immediate treatment. The hospital was small and the staff busy.
"The baby was very big and I was so young," she recalled, explaining that she experienced a prolonged, obstructed labour.
Yet she spent three days at the hospital before receiving help.
Tragically, the baby did not survive childbirth. And that was just the beginning of Ms. Kaleso’s problems.
The morning after returning home from the hospital, she woke up and noticed her bedding was wet with urine.
Ms. Kaleso had developed an obstetric fistula, an injury caused by childbirth complications. Fistula causes incontinence and can also lead to infections, chronic pain and other problems.
‘I was too young to live this life’
"I thought it was normal, but this occurred for almost a year,” she told UNFPA.
Like many fistula survivors, Ms. Kaleso suffered stigma and isolation. Her friends turned away when she approached them.
Her hopes of going back to school after delivery faded.
Ms. Kaleso said life became unbearable.
“I did not even know if this condition could be treated or not,” she recalled. “I was too young to live this kind of life.”
But one day, as Ms. Kaleso's father harvested his tobacco crop, he heard on the radio that fistula treatment was available at the Bwaile Centre in Lilongwe.
Soon after, Ms. Kaleso underwent successful surgerical fistula repair.
Back to school
UNFPA data show that 0.6 per cent of women aged 15 to 49 were living with this condition as of 2016 in Malawi. UNFPA has supported treatment for over 1,500 women in the country since 2011.
Many of these repairs have taken place through a partnership with the Bwaile Centre, which has a specialist surgeon and programme that helps survivors reintegrate into the community after treatment.
Ultimately, UNFPA and Malawi aim to transition from fistula repair to prevention. The condition is easily prevented through access to emergency obstetric care – usually in the form of a Caesarean section. In fact, fistula is so preventable that it has been essentially eliminated in industrialized countries.
Ms. Kawelo is now an ambassador for the Bwaile Centre. She helps seeks out other fistula survivors and helps them access treatment.
She has also been able to return to school. Her new dream is to finish her degree in education and teach mathematics.
“I consider myself very lucky," she said. "Some women have lived with this condition for more than 40 years, and others even 50 years or more.”
For Won Young Hong, UNFPA’s representative in Malawi, Ms. Kawelo's story demonstrates why adolescent girls need access sexual and reproductive health information and services.
“One pregnancy can have life-threatening consequences, such as HIV and other sexually transmitted diseases, birth injuries including fistula, more children, and they are at risk of dropping out of school, and thus perpetuating the cycle of poverty,” Ms. Hong said. “It is encouraging to see that Monica is back in school and pursuing her dreams”.
– Henry Chimbali
"My grandchildren will play with me. I am clean. I can practice my faith. I can live" - A fistula surviver rejoices
Watch the video"My grandchildren will play with me. I am clean. I can practice my faith. I can live" - A fistula surviver rejoices
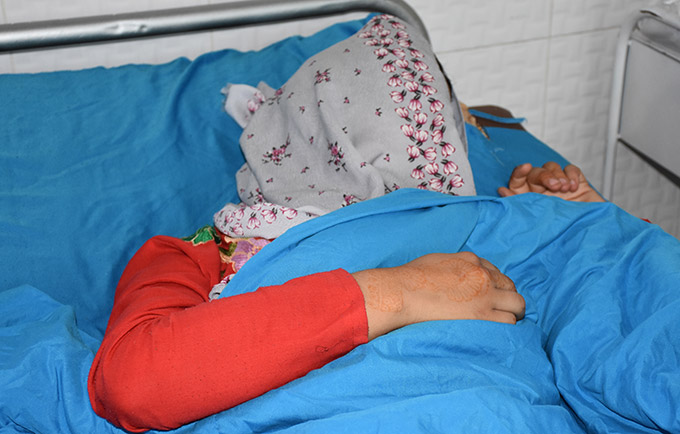
KABUL, Afghanistan – “I saw myself as the living dead,” 50-year-old Laila* told UNFPA. She suffered terribly while giving birth in Pakistan 27 years ago. The prolonged, obstructed labour left her with an obstetric fistula – one of the most serious injuries that can occur during childbirth.
Read MoreKABUL, Afghanistan – “I saw myself as the living dead,” 50-year-old Laila* told UNFPA. She suffered terribly while giving birth in Pakistan 27 years ago. The prolonged, obstructed labour left her with an obstetric fistula – one of the most serious injuries that can occur during childbirth.
The fistula – hole between the birth canal and bladder or rectum – can cause pain and chronic infections. It also causes incontinence, which often leads to women’s social isolation.
Yet the injury has been eliminated in much of the world through modern emergency obstetric care. Those who continue to suffer from obstetric fistula tend to be among the most marginalized and vulnerable.
“At the beginning, I was ashamed to tell anyone that I had fistula. Most of the time, I could not take part in social gatherings because I smelled bad,” Laila recounted.
As can be the case for fistula survivors, Laila lived with the injury for decades.
According to a 2015 survey, approximately 3 per cent of ever-married Afghan women have experienced obstetric fistula. Contributing to this high prevalence are the country’s high rates of child marriage and adolescent birth – early childbearing increases the risk of complications.
Poor access to health services also plays a key role. Only 51 per cent of births in Afghanistan take place with the help of a skilled birth attendant.
But there is help.
Years ago, Laila moved from Pakistan to Paghman Province in Afghanistan. Then one day she learned about the Malalai Maternity Hospital in Kabul, where surgical fistula repair is available.
Afghanistan’s only expert fistula repair surgeon works at the Malalai centre, along with four additional surgeons who provide basic fistula operations.
The treatment was a success, she says. “The operation has given me a new life," she said.
Twenty-year-old Farah* also suffered a prolonged labour during childbirth at her home in Afghanistan’s Faryab Province six months ago.
“My life became very hard. I could not talk to anyone about my condition because of shame,” she recounted to UNFPA. “It made my life completely unbearable.”
The injury caused pain and bleeding, as well.
“I could not work, sleep or walk as I did before. I was not able to go out because of bleeding. I was not able to sit on the ground, on chairs or on carpets because of my illness.”
She isolated herself. “I could not gather with my relatives and family members because of my bad smell. I was fed up of my life. I should have been working in the home with cooking, cleaning and doing laundry as a housewife but was not able to do any of that properly. I felt incapable and useless in society.”
Fortunately, her family stood by her.
“They knew that I had fistula but they never changed their behaviour towards me. They never left me to suffer alone,” she said.
Not long ago, one family member learned about the Malalai fistula centre and helped Farah get treatment.
“I am happy, healthy and hopeful again after the operation,” she said. “I am a capable member of society once more and can start over with my child, husband and family members and live a normal life.”
UNFPA helped to establish the Malalai fistula treatment centre in 2007, and continues to provide support to its operations. UNFPA covers the cost of treatment, medication and transport for patients, and supports training for the hospital’s expert fistula surgeon.
There are also four additional surgeons providing fistula repair in two other provinces, Herat and Jalalabad. Since 2010, more than 600 surgical fistula repairs have taken place in collaboration with the Afghan Ministry of Public health, including 45 this year.
Still, across the country there is a major shortage of surgeons able to perform these operations. In addition, rehabilitation and reintegration programmes – which can help survivors overcome social isolation – are not available.
Farah wants to help other women avoid her ordeal.
“I would like to encourage every woman suffering from obstetric fistula to seek help without any concern and shame,” she said. “I also want to tell them to be careful not to go through childbirth without a skilled birth attendant to assist during delivery.”
*Names changed for privacy reasons