News & Updates
Obstetric fistula stories and announcements
Obstetric fistula stories and announcements

Every year on 23 May, the International Day to End Obstetric Fistula is observed by the international community as a way to rally action, commitment and support to ending obstetric fistula.
Read MoreEvery year on 23 May, the International Day to End Obstetric Fistula is observed by the international community as a way to rally action, commitment and support to ending obstetric fistula.
In December 2012, 167 countries co-sponsored a biannual resolution of the United Nations General Assembly that called on all Member States to support UNFPA and its partners in the Campaign to End Fistula. In addition, the UNFPA-backed resolution acknowledged the plight of millions of women and girls living with obstetric fistula by designating 23 May as the International Day to End Obstetric Fistula, first observed in 2013.
Subsequent resolutions have called for the dramatic acceleration of actions and commitment to end obstetric fistula by 2030, reinforcing the need for urgent efforts and greater investment to address and improve sexual and reproductive, maternal, newborn and child health, as well as to eliminate the root causes of fistula, such as poverty, inequalities and failure to ensure education, economic opportunity, gender equality and human rights for all.
A sign of global social injustice and inequity stemming from weak health and social protection systems, obstetric fistula is driven by poverty, gender and socioeconomic inequality, lack of education, child marriage and early/adolescent childbearing, among other things. Women and girls at risk of or living with fistula face economic, social, cultural and logistical barriers to care and to survival, further deepening pre-existing inequalities.
The condition is generally and often treatable, but more critically, it is largely preventable – developed countries have all but eliminated obstetric fistula. The same should be true for developing countries. Everyone deserves a life of dignity, and the day serves as a reminder that we cannot ignore such a promise.
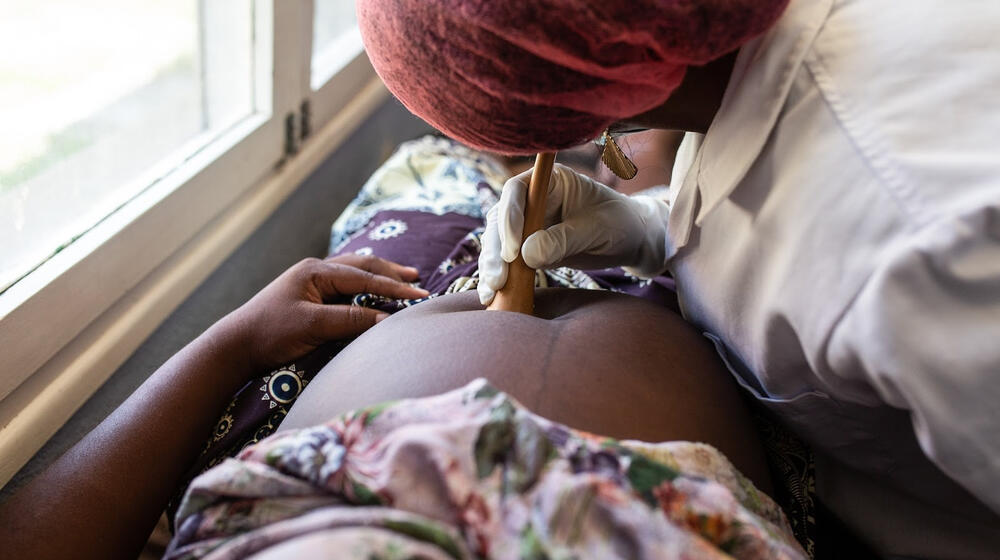
UNITED NATIONS, New York – First things first, what is obstetric fistula?
What it is: Obstetric fistula is a traumatic childbirth injury that robs a woman or girl of her health, rights and dignity. It is a hole between the birth canal and bladder that causes uncontrollable urinary incontinence. A hole between the birth canal and rectum causes faeces to leak.
Read MoreUNITED NATIONS, New York – First things first, what is obstetric fistula?
What it is: Obstetric fistula is a traumatic childbirth injury that robs a woman or girl of her health, rights and dignity. It is a hole between the birth canal and bladder that causes uncontrollable urinary incontinence. A hole between the birth canal and rectum causes faeces to leak.
Why it happens: Prolonged, obstructed labour during childbirth. The sustained pressure of a baby’s head against the mother’s pelvis cuts off blood supply, causing tissue to die and fall away; the hole left is called a fistula. Obstetric fistula accounts for eight per cent of maternal deaths, and 90 per cent of all cases in which a fistula occurs, result in stillbirth.
Who it affects and where it happens: An estimated 500,000 women and girls in more than 55 countries throughout sub-Saharan Africa, Asia and the Pacific, the Arab States and Latin America and the Caribbean are estimated to be living with fistula, with thousands more occurring every year.
Below, five more things you should know:
While the most common type is a hole between the birth canal and bladder (called vesicovaginal fistula), other types include:
Rectovaginal fistula: Hole between birth canal and rectum
Urethrovaginal fistula: Hole between birth canal and urethra (carries urine from bladder out of the body)
Ureterovaginal fistula: Hole between birth canal ureters (carry urine to bladder) and birth canal
Vesicouterine fistula: Hole between bladder and uterus
Some fistulas are caused during gynaecological procedures (e.g. hysterectomy) and Caesarean sections due to substandard health care and inadequate surgical skills training/competence. These are called iatrogenic fistulas. Traumatic fistulas are caused by sexual violence, especially in conflict areas; the destruction of the vagina is considered a war injury.
The lives of women with the condition are defined by lifelong physical and emotional suffering.
The condition can lead to infections, ulcerations, kidney disease, painful sores, infertility and death. The smell from constant leakage isolates women who are often shamed and stigmatized, abandoned by their friends and families and ostracized by their communities. They suffer from depression and suicidal thoughts and other mental health issues. Denied livelihood opportunities, they are driven deeper into poverty and vulnerability.
While it does not discriminate by age, young girls are particularly vulnerable because their bodies may not be ready for childbirth. Nine in ten births to girls between the ages of 15 and 19 occur in marriage or union. Worldwide, pregnancy and childbirth complications are the leading cause of death among girls between the ages of 15 and 19. It’s just one more reason UNFPA works to eradicate the harmful practice of child marriage.

Obstetric fistula has all but disappeared in rich countries with quality health care systems and skilled professionals who can perform Caesarean sections. Midwives are a vital part of the solution. The International Confederation of Midwives states “ending obstetric fistula requires the full involvement of midwives at the community, national, regional and global levels.”
Apart from a lack of quality health services, poverty is a major social risk because it is associated with early marriage and malnutrition. Childbearing before the pelvis is fully developed as well as malnutrition, small stature and generally poor health conditions are contributing physiological factors to obstructed labour. However, older women who have already had babies are at risk as well.
In addition, because of gender inequality in many communities, women don’t have the autonomy or agency to decide when to start having children or where to give birth.
Up to 95 per cent of fistulas can be closed with surgery. A surgical repair costs $600, well beyond the reach of most women with fistula – if they’re even aware of the exact medical condition they have and that treatment exists. Through its assistance to countries and the Campaign to End Fistula UNFPA has supported more than 121,000 life-changing repairs since 2003 and trained thousands of health workers to prevent and treat fistula.
But before ever reaching the treatment stage, focus should be on prevention. Such measures include access to family planning, skilled birth attendants and emergency obstetric care. Addressing societal factors that contribute to fistula – child marriage/early union and pregnancy, girls’ education, poverty and women’s lack of empowerment – is also part of the Campaign to End Fistula strategy.
To have one’s life compromised for bringing forth new life is a devastating fate. But with awareness and will, the goal of eradicating the condition by 2030 is achievable.
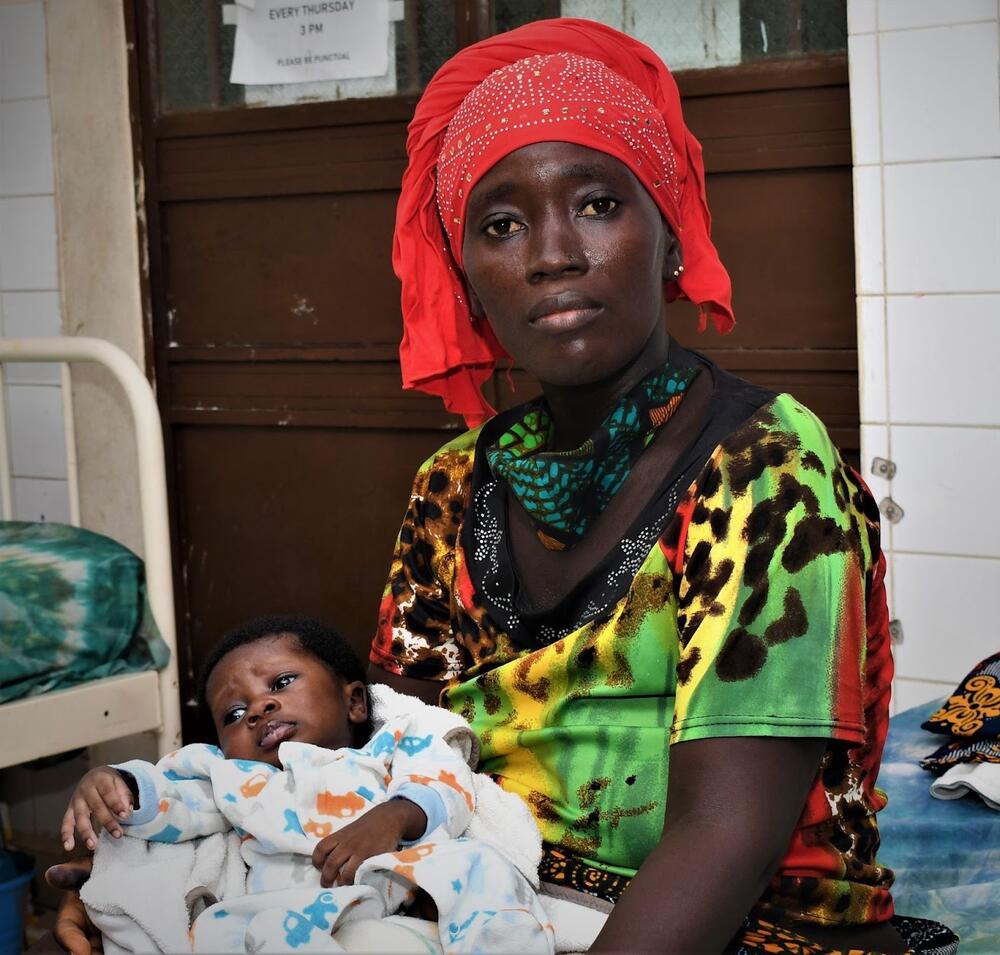

UNITED NATIONS, New York – Celebrated around the world throughout the year, Mother’s Day is exactly that: celebratory. But for some women, motherhood can be fraught.
Read MoreUNITED NATIONS, New York – Celebrated around the world throughout the year, Mother’s Day is exactly that: celebratory. But for some women, motherhood can be fraught. Women have become mothers below ground in wartime (Ukraine), under bridges after hurricanes (Honduras), in flooding hospitals during monsoon season (Bangladesh) and among post-earthquake wreckage (Haiti).
They have become mothers not by choice, but…:
…against their will as a result of rape – by a partner or stranger – or where sexual violence is used as a weapon of conflict.
…because it is expected of them by their cultures and families, even if they are not physically or emotionally ready for pregnancy.
…without knowing how conception works due to a lack of comprehensive sexual education. And when they do know, they have become mothers because of a lack of access to adequate family planning services.
Parenthood comes with sacrifices, no doubt. Even before mothers left the workforce in droves during COVID-19 to care for children attending school remotely, they were already shouldering much of the burden for child-rearing, housework, emotional labour and caring for ageing parents. They may have had to forego higher degrees, promotions or relocations. If they return to work after raising children, they may have outdated skills and face the “motherhood pay gap.” With long retirements due to longevity, their “choices” may leave them in precarious financial situations.
But the steepest price some women pay for becoming pregnant is never having the chance to experience motherhood. The global maternal mortality ratio is 211 deaths per 100,000 live births in 2017. The Sustainable Development Goals call for reducing that number to 70 deaths per 100,000 live births by 2030.
Below, five things to know about motherhood.
It’s not surprising that everything is harder in humanitarian or fragile contexts. In regards to fertility, women must contend with everything from becoming pregnant when they might not want to – because of limited access to family planning services and contraception or because of the increased risk of gender-based violence in these settings – to challenging pregnancies and childbirth due to a lack of antenatal and postnatal care and obstetric care. According to a UNFPA report, more than 500 women and girls die in emergency situations every day from complications due to pregnancy and childbirth. In conflict-roiled Yemen, a woman dies in childbirth every two hours. Approximately 120,000 pregnant and lactating women in Tigray, Ethiopia are malnourished. About 4.8 million unintended pregnancies will occur in Afghanistan by 2025 as a result of health system disruptions and gender inequality.
According to the 2017 Fragile States Index, 15 countries were considered to be “very high alert” or “high alert” (from highest to lowest: South Sudan, Somalia, Central African Republic, Yemen, Syrian Arab Republic, Sudan, the Democratic Republic of the Congo, Chad, Afghanistan, Iraq, Haiti, Guinea, Nigeria, Zimbabwe and Ethiopia), and these 15 countries – the majority considered humanitarian and fragile contexts – had maternal mortality ratios as high as 1,150 (South Sudan). For countries, the target is no more than 140 deaths per 100,000 live births by 2030.
As the report states, “Emergent humanitarian settings and situations of conflict, post-conflict and disaster significantly hinder progress… In crisis and disaster settings, the breakdown of health systems can cause a dramatic rise in deaths due to complications that would be easily treatable under stable conditions.”
Another non-shocker: women do more unpaid work than men.
A 2019 report from the International Labour Organization (ILO) puts it bluntly: “Across the world, without exception, women carry out… more than 75 per cent of the total hours [of unpaid care work] provided. Women dedicate on average 3.2 times more time than men to unpaid care work. There is no country where women and men perform an equal share of unpaid care work. As a result, women are constantly time poor, which constrains their participation in the labour market.”
Globally, in households with young children, women spend more time on unpaid care work. In 2018, mothers of children 5 years old and younger accounted for the lowest employment rates (47.6 per cent) compared with fathers (87.9 per cent), non-fathers (78.2 per cent) and non-mothers (54.4 per cent).
A sizeable reason for the disparity is gender inequality overall. According to the ILO, the value of women’s unpaid care work accounts for 6.6 per cent of global GDP, or $8 trillion; that number for men represents 2.4 per cent of global GDP, or $3 trillion.
Under Sustainable Development Goal 5 of Gender Equality is Target 5.4 – the recognition and valuing of unpaid care and domestic work – to be achieved by 2030.
According to the World Health Organization, five major complications – many preventable or treatable – account for three quarters of maternal deaths: severe bleeding, infections, high blood pressure during pregnancy, complications from delivery and unsafe abortion.
Other causes merit more examination, namely maternal deaths as a result of homicide, suicide and drug overdose. In the United States, one study reported all three as leading causes of pregnancy-associated* deaths, with homicide rates higher than in other countries. In the UK and Ireland, one report concluded that improvements in care might have led to different outcomes in pregnancy-associated deaths by suicide, substance misuse and homicide. And studies in Ethiopia and Egypt found higher prevalence of suicidal behaviour among pregnant women compared to the general population.
*A pregnancy-related death is “‘the death of a woman while pregnant or within one year of the end of a pregnancy… from any cause related to or aggravated by the pregnancy or its management, but not from accidental or incidental causes.’... A pregnancy-associated death is a maternal death attributable to a condition unaffected by the pregnancy and occurs within one year of the pregnancy.”
According to the 2022 State of World Population report, rape-related pregnancies are equally or more likely to occur than pregnancies from consensual sex. In addition, intimate partner violence (IPV) is linked to higher rates of pregnancy. Those experiencing IPV are roughly twice as likely to have their partner refuse to use contraception and twice as likely to report an unintended pregnancy.
If we did, wouldn’t we eradicate childbirth injuries like obstetric fistula?
Wouldn’t we support mothers suffering from postpartum mental health issues?
Wouldn’t every new mother be given proper time to bond with her child and recover her health without risk of losing her job?
Wouldn’t we not assume that all women everywhere are destined to become mothers, thereby devaluing motherhood as an inevitability rather than an aspiration?
Wouldn’t child care and domestic responsibilities be evenly divided?
And wouldn’t we truly make motherhood a choice by giving women and girls the information, resources and support they need: Access to sexual and reproductive health services, comprehensive sexuality education, family planning services and contraception, access to higher education and economic opportunities, protection from violence and above all, gender equality that would render the world safer, healthier and more prosperous not only for them but for everyone.

Ntchisi, Malawi-Although Marita Vula was in pain, she tried as much as possible to ignore it. The 28-year-old was experiencing her first labour pains.
Read MoreNtchisi, Malawi-Although Marita Vula was in pain, she tried as much as possible to ignore it. The 28-year-old was experiencing her first labour pains. Marita had waited for this moment and couldn’t wait to a be a mother.
“When I got married, I stayed for three years without a child,” says Marita from Kambola village in Ntchisi. “In our culture, one is expected to have a child as soon as they get married.”

However, try as they could, Marita couldn’t get pregnant. This displeased her in-laws who took every opportunity to remind her that they wanted grandchildren.
On this particular day, Marita’s husband was tending their maize field. When he heard the news that her wife was in labour, he hurried back home. Since the hospital was too far, he decided to take Marita to a traditional birth attendant to help her deliver.
“That was the only option we had that time,” recalls Marita, adding, “I didn’t see the labor coming that soon and hadn’t planned to travel to the hospital.”
Access to maternal services still a challenge
For hours, the traditional birth attendant tried to help Marita to deliver but without luck. In desperation, the traditional birth attendant prepared some herbs, which she said would help ‘push the baby out’. Instead of helping her give birth, the herbs made Marita lose a lot of blood.
“My husband became worried and he rushed to the nearby village to hire a car,” she said. “When he came back, I had passed out. The next thing I remember was in a hospital. The look on my husband face told me that something terrible had happened.”
Marita arrived at the hospital semi-conscious. Medical staff had to perform a caesarian section to save both mother and child. Unfortunately, the child didn’t make it. Her husband had to break the sad news to her.
“This was devastating news. I was looking forward to holding my child in my hands,” says Marita.
Although Marita recovered well, she could no longer control her urine and she kept wetting herself. The prolonged labour caused her to develop a hole between the birth canal and the bladder. As a result, she developed obstetric fistula.
“When I returned home, my husband’s attitude towards me changed,” she says. “He started sleeping in his own bed.”
A ray of hope for women with fistula
For eight months, nothing changed. Eventually, her husband disappeared only for Marita to learn that he had married in another village.
“I was okay with him sleeping on another bed,” she says. “But running away from me was the last thing I expected from him. He was responsible for the pregnancy and I couldn’t have developed fistula if it wasn’t for him.”

With time, Marita soon learnt to accept her condition. One day, as she was listening to the radio, she had a testimony of a woman who was successfully treated of fistula. She listened with interest and learnt that the operation was done at Bwaila Fistula Centre in Lilongwe.
Marita saved enough money for transport to seek for treatment at the Centre. The waiting list was long. She stayed at the Centre for a month and finally got repaired of fistula.
Helping fistula survivors reintegrate in society
“The support I received from the fistula centre transformed my life,” says Marita, who is now a fistula ambassador in her community. “I have moved from being a social outcast to become one of the community respected tailors.”
As one way to help her reintegrate in her community, the Bwaila Fistula Centre with support from the European Union funded Spotlight Initiative, trained Marita and other 48 fistula ambassadors in tailoring. The ambassadors’, including Marita, were each given a sewing machine to help them establish tailoring shops for income generation.
Today, Marita is a well-known tailor in her community. She sews’ dresses, suits and all type of uniforms. In a good month, Marita makes about US$80. And when its wedding season, her earnings goes up to more than US$100 per month, she says.
“I am saving money to buy iron sheets for my house,” she says. “I have lived a difficult life and now just want to make the best of what I have.”

In 2021, UNFPA successfully lobbied for the re-opening of the Bwaila Fistula Centre after it was converted into a Covid-19 isolation centre. The closing of the Centre inconvenienced hundreds of women suffering from fistula from getting treatment. Since re-opening, the Centre with support from the Spotlight Initiative, has successfully repaired 90 women suffering from fistula.
Joseph Scott, Communication Analyst
The Ministry for Foreign Affairs of Iceland and UNFPA have signed a $7 million landmark agreement to help end obstetric fistula in Sierra Leone and improve the lives of the women and girls suffering from this preventable condition. Sierra Leone has one of the highest lifetime risks of pregnancy-related mortality and morbidity, including obstetric fistula.
Read MoreThe Ministry for Foreign Affairs of Iceland and UNFPA have signed a $7 million landmark agreement to help end obstetric fistula in Sierra Leone and improve the lives of the women and girls suffering from this preventable condition. Sierra Leone has one of the highest lifetime risks of pregnancy-related mortality and morbidity, including obstetric fistula.
Obstetric fistula is one of the most serious and tragic childbirth injuries. Women suffering from obstetric fistula are often stigmatized and isolated from their families and communities. They face significant socioeconomic challenges and often do not have access to social-economic development opportunities in their communities.
“Obstetric fistula is a neglected health and human rights tragedy that affects the most vulnerable women and girls. It is embedded in gender inequalities and social norms and constitutes an impediment to women and girls’ empowerment.” says UNFPA West and Central Africa Regional Director Argentina Matavel-Piccin.
In recent years, Iceland has been supporting the Government of Sierra Leone in its efforts to prevent and treat obstetric fistula, with the aim to improve access to quality maternal health services to prevent and manage obstetric fistula. This new landmark agreement will provide medium- to long-term support to end obstetric fistula in the country, and is part of the global Campaign to End Fistula launched by UNFPA and its partners in 2003.
The five-year programme will take a comprehensive and integrated approach to obstetric fistula, by addressing the gender and other social norms, and health systems challenges contributing to the occurrence of obstetric fistula. The new partnership will strengthen the referral system for surgery and social reintegration initiatives, and will focus on documenting best practices to help shape other existing and future programmes.
By the term of the programme, the capacity of the country’s health system will be strengthened to improve adolescent girls’ and women’s access to integrated sexual and reproductive health services for prevention, treatment and social reintegration of obstetric fistula.
“Iceland has been a firm supporter of the Global Campaign to End Fistula for more than a decade – both financially through UNFPA and through our advocacy efforts for sexual and reproductive health and rights at the international level,” said Thórdís Kolbrún Reykfjörd Gylfadóttir, Minister for Foreign Affairs and International Development Cooperation of Iceland. “We are very proud to be part of this programme and work together with UNFPA and the Government of Sierra Leone toward the elimination of obstetric fistula in the country.”
“Our long-standing partnership with the Government of Iceland plays a critical role in supporting UNFPA’s ongoing campaign to end obstetric fistula in Sierra Leone and globally, and in restoring women’s dignity worldwide,” said UNFPA’s Matavel-Piccin.

MOCUBA, ZAMBEZIA PROVINCE, Mozambique – Beatriz Sebastião suffered in silence. She had no friends in the neighborhood or at school. When she went to church, she sat alone. When she went to the river, other women mocked her before leaving to bathe elsewhere.
Read MoreMOCUBA, ZAMBEZIA PROVINCE, Mozambique – Beatriz Sebastião suffered in silence. She had no friends in the neighborhood or at school. When she went to church, she sat alone. When she went to the river, other women mocked her before leaving to bathe elsewhere.
She had become pregnant at 15 and because she lived far from the hospital, planned to give birth at home. After three days of labour, her parents had to raise money to rent a motorcycle to take her to the hospital, where she delivered a stillborn child. She developed an obstetric fistula, and when she became pregnant again, that child, too, was stillborn. But the fistula caused urine to leak, and the resulting smell isolated her from nearly everyone for the next six years.
A treatable, preventable condition
Obstetric fistula is a hole between the birth canal and bladder or rectum, which can cause incontinence, leading to social ostracization and attendant psychological issues like depression. The treatable and largely preventable condition is the result of prolonged, obstructed labour with no access to skilled care, often resulting in stillbirth. Girls whose bodies are too young to deliver a baby are particularly vulnerable.
Every year, there are an estimated 2,500 reported fistula cases in Mozambique, of the 50,000 to 100,000 cases globally. Since 2018, in partnership with the Government of Mozambique, UNFPA has supported the repair of more than 2,300 fistulas, recruited 28 fistula surgeons, expanded a real-time monitoring system of cases to 25 health facilities, and educated thousands of people about the causes and consequences of the condition.
A life transformed
Ms. Sebastião, now 28, had once sung gospel and six years after developing the fistula, received a fateful invitation to perform at a youth meeting. Encouraged by an uncle, she went, “but as always, I was discriminated against. I was humiliated. People talked. Because of the looks, I stayed there shrunken.” She stayed alone in a tent because no one would share space with her.

Then the youth coordinator, who also worked at a hospital, sought her out when she skipped practice, claiming illness. Finally, she admitted she had “a disease that made me pee involuntarily,” which is when she learned that what she had could be cured through surgery.
Ms. Sebastião was one of the rare fistula survivors whose family and husband did not abandon her. With their support, she had the operation and, for the first time in years, awoke without having wet the bed. “I don’t know how to express what was in my heart,” she recalled. “I had emotions I don’t know how to describe.”
She was no longer the person others fled from. She could wear skirts again, instead of covering herself with multiple layers of cloth. She started a small grocery business, something unthinkable before, and became an activist, holding chats with women in various communities to discuss fistula. She learned “to love that Beatriz from the past again,” she said. “When I had the disease, I was nothing. Now, I am capable of everything, able to fight for my well-being and raise my self-esteem.”
The contagious joy of a woman with a repaired fistula
Albertina Luis is a radio journalist and activist in Mocuba District. When her activism focused on domestic violence, she would meet women hiding behind their houses or in the cassava trees – not from abusive husbands but because they had obstetric fistulas. Ms. Luis underwent reproductive sexual health training and learned more.

Now, through regular broadcasts, she reduces shame and stigma surrounding obstetric fistula and lets women know how to prevent it, including avoiding forced, premature marriage and unintended pregnancy, and where to seek medical treatment. “Dignity means being valued,” Ms. Luis, 50, said. “The greatest wealth is health. In addition to being a right, it is power. I am freeing women who have lost their dignity for a long time.”
Dr. Armando Rafael, a fistula surgeon at Mocuba Rural Hospital, who operated on Ms. Sebastião, finds his work rewarding, knowing the suffering and marginalization patients have endured. “The contagious joy of a woman when her fistula is repaired is incomparable,” he said.
During Ms. Sebastião’s long exile, women at the river taunted her with the cruel nickname “Lake Bethesda,” a reference to the Bible's Pool of Bethesda that never ran dry. For her, the name takes on a different significance now: in Biblical lore, the pool was a place where miracles happened and people were healed.

BOUAKÉ, Côte d'Ivoire
Read MoreBOUAKÉ, Côte d'Ivoire – When Blandine was pregnant, she didn't go to the hospital for regular prenatal check-ups. On the day she gave birth, she delayed in going to the health centre. Her doctor told her that's why the birth had complications which resulted in her developing obstetric fistula.
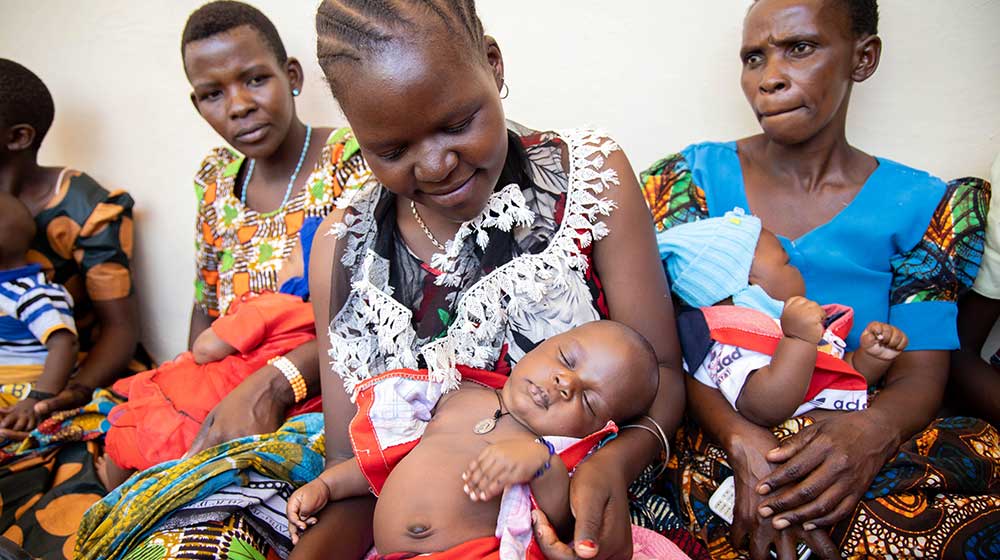

The most vulnerable women
Under the shadow of war
Support needed

ISLAMABAD, Pakistan – “Helping women suffering fistula is my mission in life," Razia Shamshad said about the maternal injury from childbirth that she thought would ruin her life. “No woman deserves to live in misery, especially when it is treatable.”
Read MoreISLAMABAD, Pakistan – “Helping women suffering fistula is my mission in life," Razia Shamshad said about the maternal injury from childbirth that she thought would ruin her life. “No woman deserves to live in misery, especially when it is treatable.”
Ms. Shamshad, 29, was born in a small village in southern Punjab. Her family did not want her to go to school, so she had only received an informal religious education by age 13, when she was married off. Ms. Shamshad was already expecting her first baby within a few weeks of her wedding. Then, when she was six months pregnant, her husband died in a road accident.
Unable to afford proper medical care, Ms. Shamshad was assisted by an unskilled traditional birth attendant who was unable to manage complications. When Ms. Shamshad suffered an obstructed labour, the birth attendant did not summon medical help. Ms. Shamshad was in agony for four days, an ordeal that could have killed her.
In the end, her daughter was stillborn, and Ms. Shamshad suffered serious damage. She developed an obstetric fistula, a hole in the birth canal. Fistula leaves women leaking urine, faeces or both, and often leads to chronic medical problems.
The condition is preventable with timely access to quality medical care, such as Caesarean section. Tragically, it persists among the most marginalized women, with pregnant adolescents and undernourished women facing particularly high risks. And its sufferers are further marginalized, often facing ostracism and discrimination.
"People would either avoid me or just make fun of me," she said. "I never felt clean."
But Ms. Shamshad was able to put her life back together. Her relatives learned about free treatment available at the Koohi Goth Women’s Hospital, which specializes in treating fistula and other conditions related to reproductive health. Two years after her ordeal, her family paid for her to travel to Karachi for care.
Ms. Shamshad’s condition was complex, and required multiple surgeries between 2010 to 2016. Even so, she has been able to regain her life.
“Her determination was exceptional. She was resilient and strong and was able to pull through the difficult process successfully,” said Dr. Sajjad Ahmed, who was trained by UNFPA to perform fistula repair surgeries.
Ms. Shamshad went on to meet her current husband. They adopted a little girl. And though she was not expected to be able to get pregnant again, she surprised everyone by conceiving. With regular prenatal care and a C-section, she had a healthy baby girl.
In many ways, Ms. Shamshad was lucky. The story is very different for many fistula survivors in Pakistan, who are unaware that there is treatment available.
And many more women and girls are at risk. Access to reproductive health services remains a challenge for women in Pakistan. Only an estimated 52 per cent of women give birth with the help of a skilled attendant, leaving them vulnerable to complications like prolonged, obstructed labour.
In partnership with the Pakistan National Forum on Women's Health, UNFPA has established treatment centres for fistula patients across the country. UNFPA also supports campaigns to raise awareness about the importance of skilled obstetric care and ending the stigmatization of women with fistula.
UNFPA leads the global Campaign to End Fistula. Since 2003, UNFPA has helped perform over 105,000 surgical fistula repairs in more than 55 countries in Africa, Asia, the Middle East and Latin America.
Today, Ms. Shamshad lives with her family in Karachi. She volunteers at the same hospital where she received the treatment that turned her life around. Ms. Shamshad helps new patients recover after their own treatment.
“I believe life experiences shape us into the people we need to become," she told UNFPA. "My experiences have given me the courage and drive to help women who have lost all hope because of fistula.”
Ms. Shamshad recently represented the hospital at the Nairobi Summit on ICPD25 in November 2019. She used her story to inform and motivate other women, to whom she has proven to be a source of encouragement.
"Never give up hope," she told them.